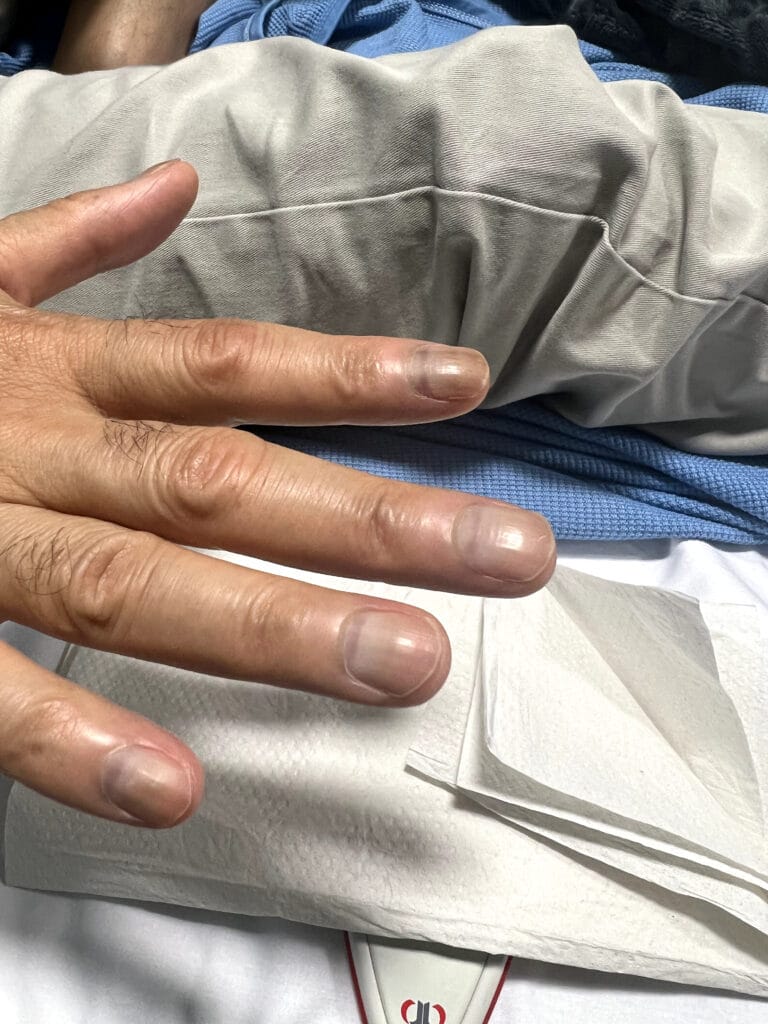
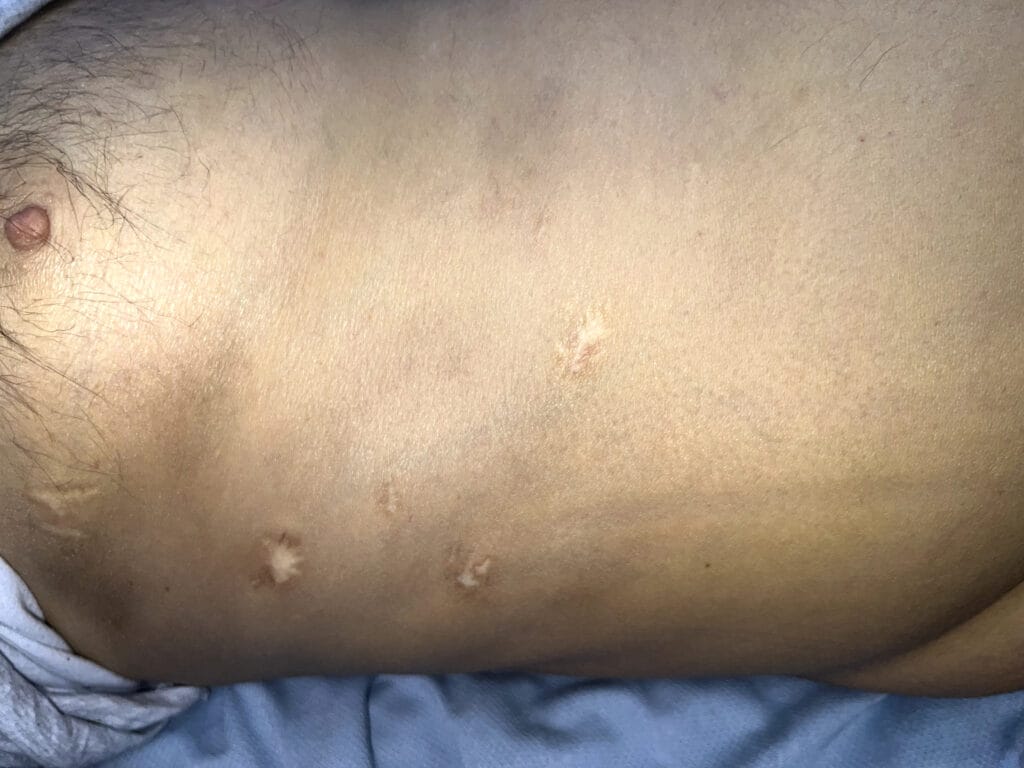
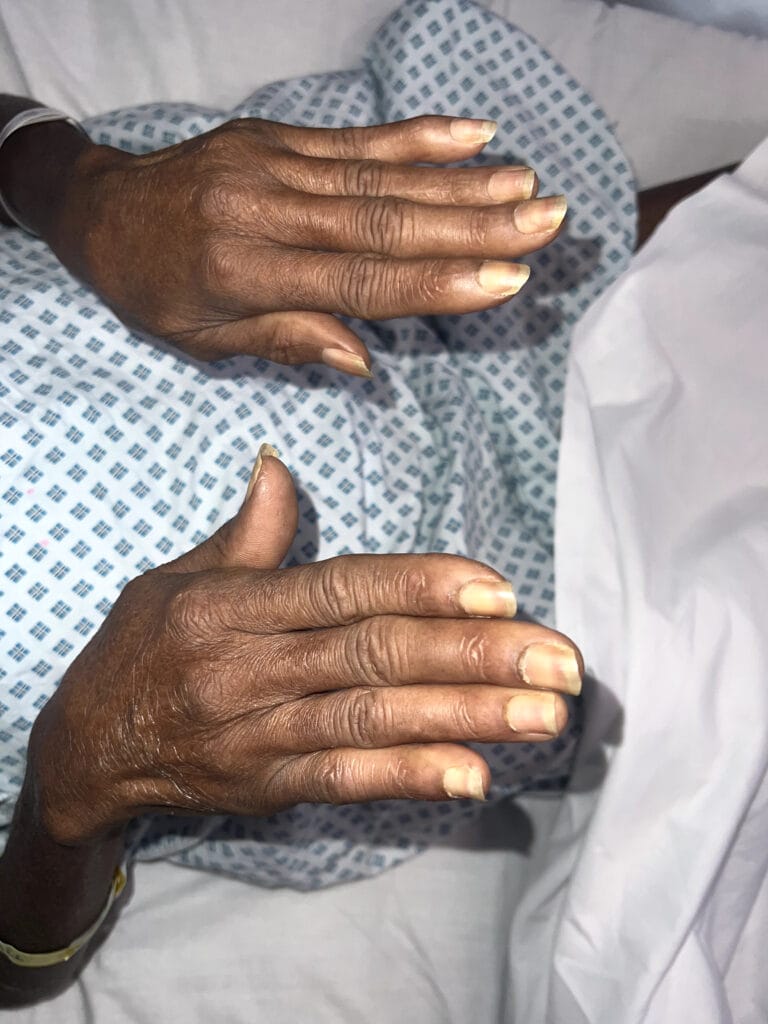
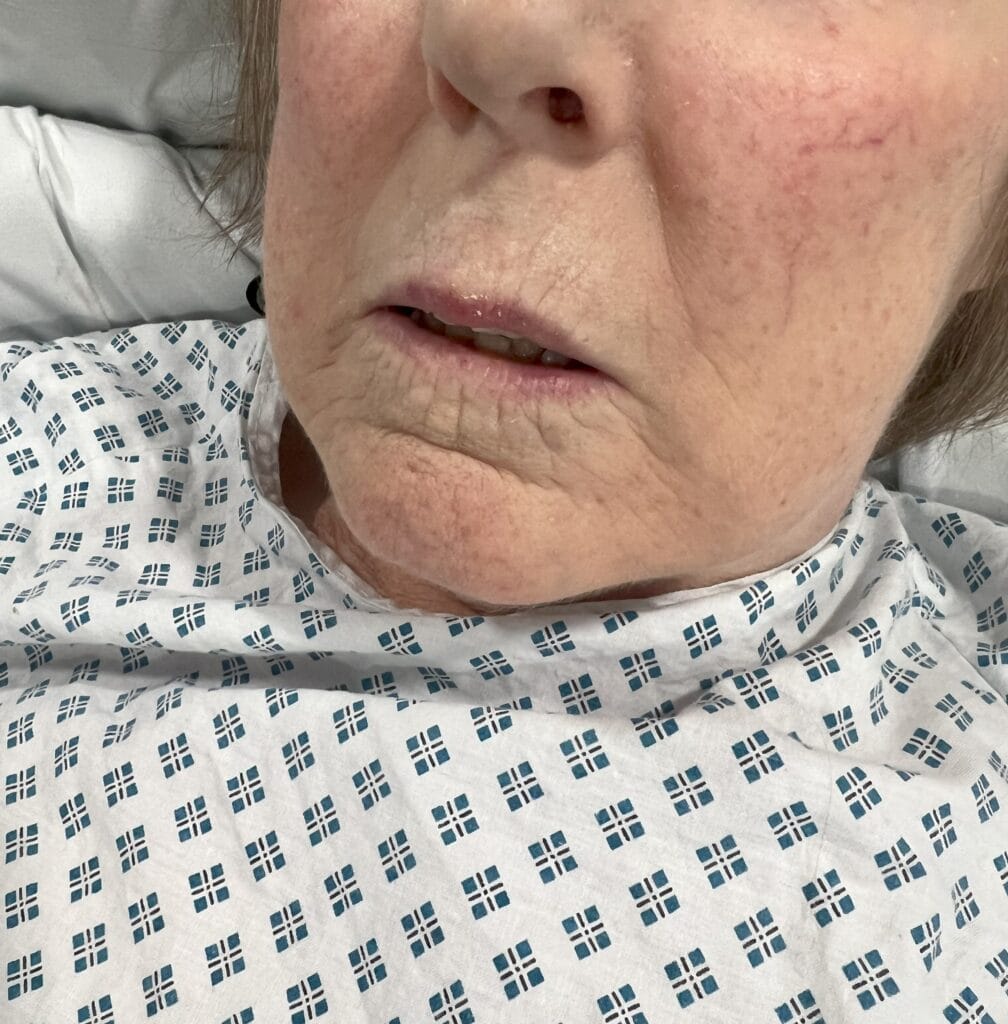
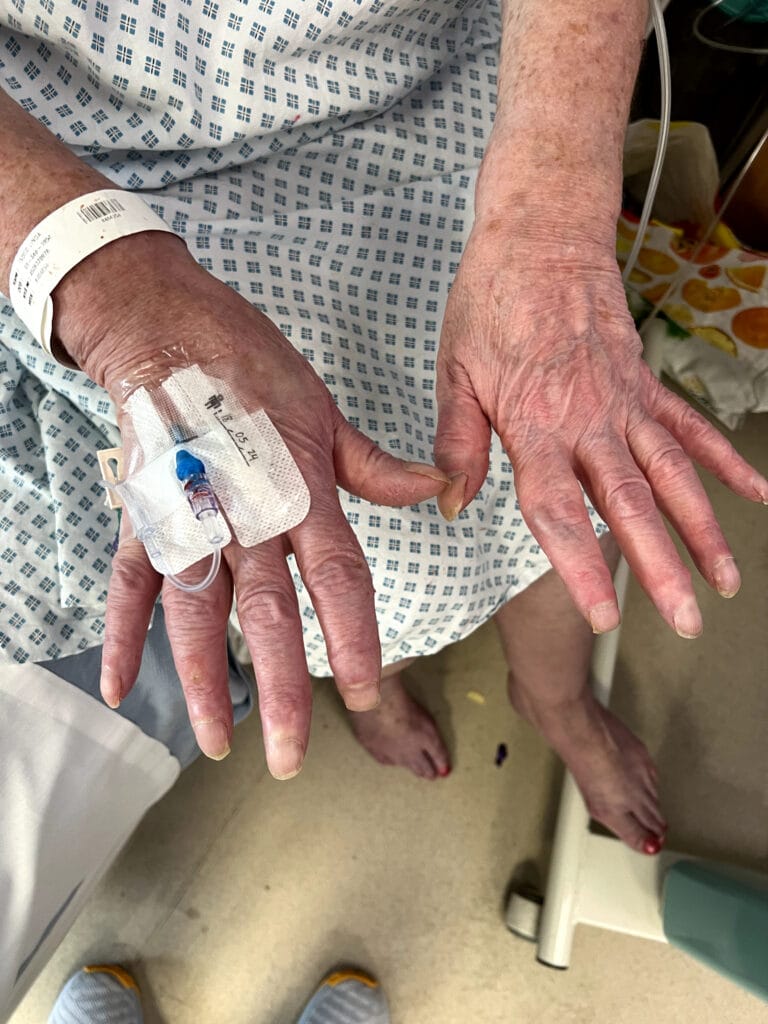
Neurofibromatosis
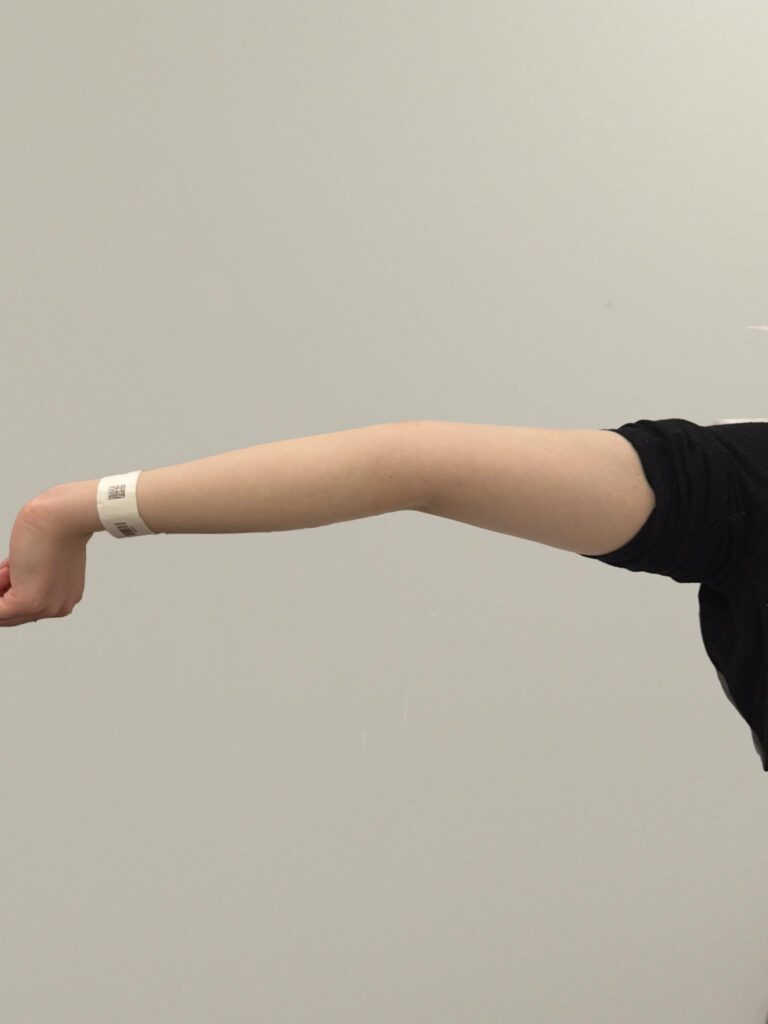
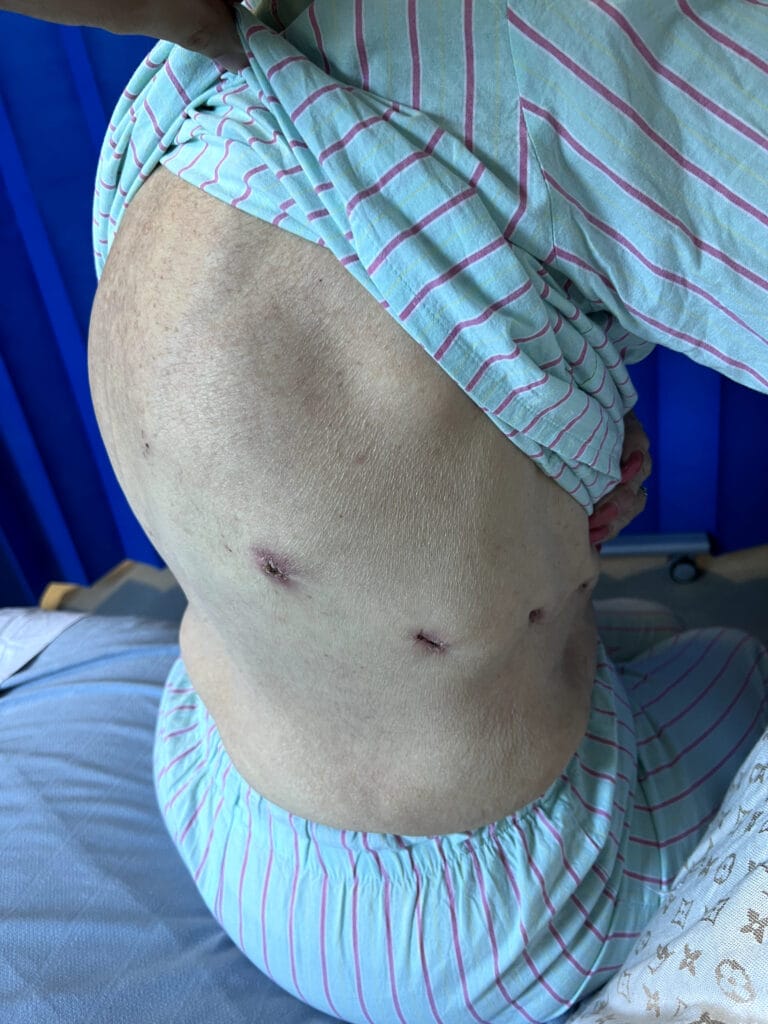
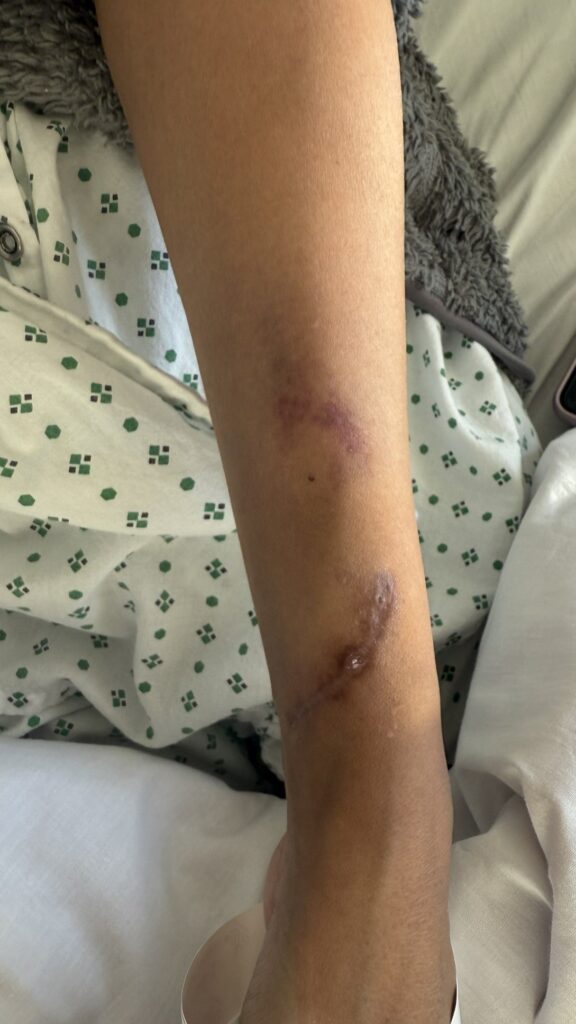
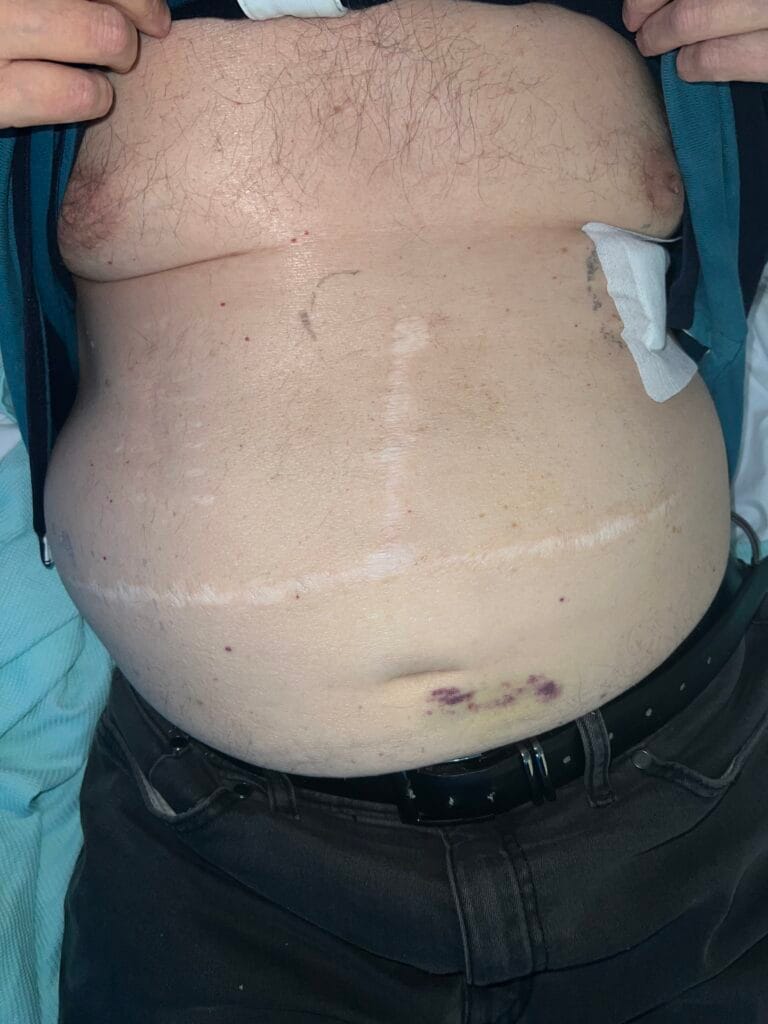
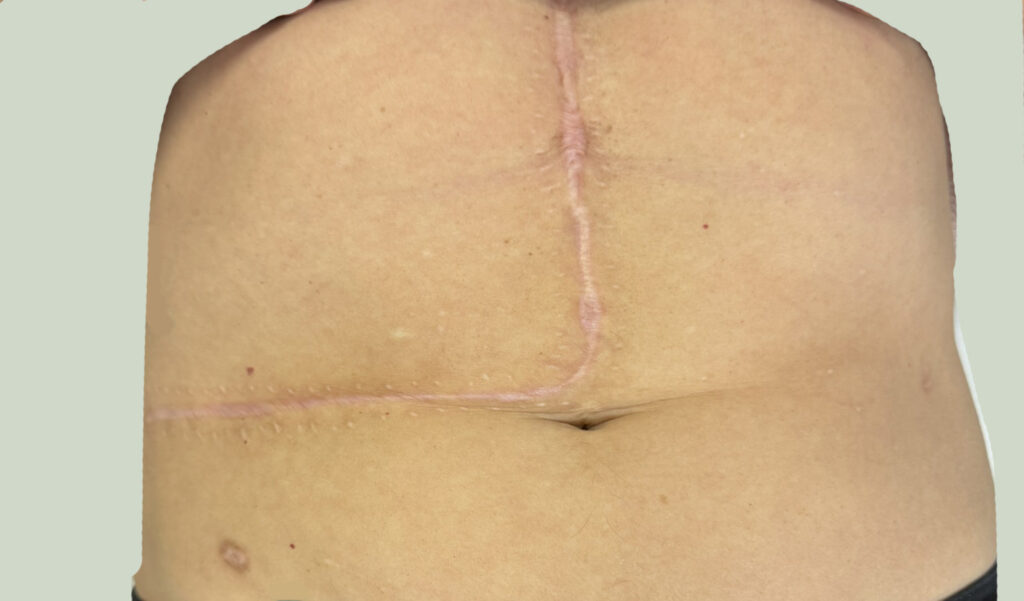
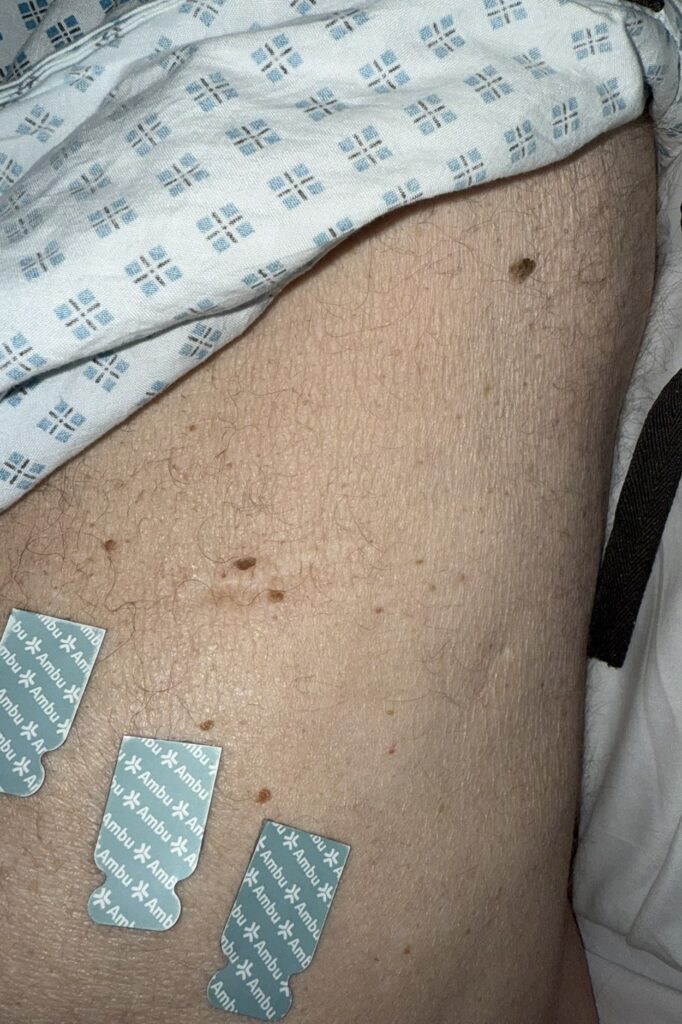
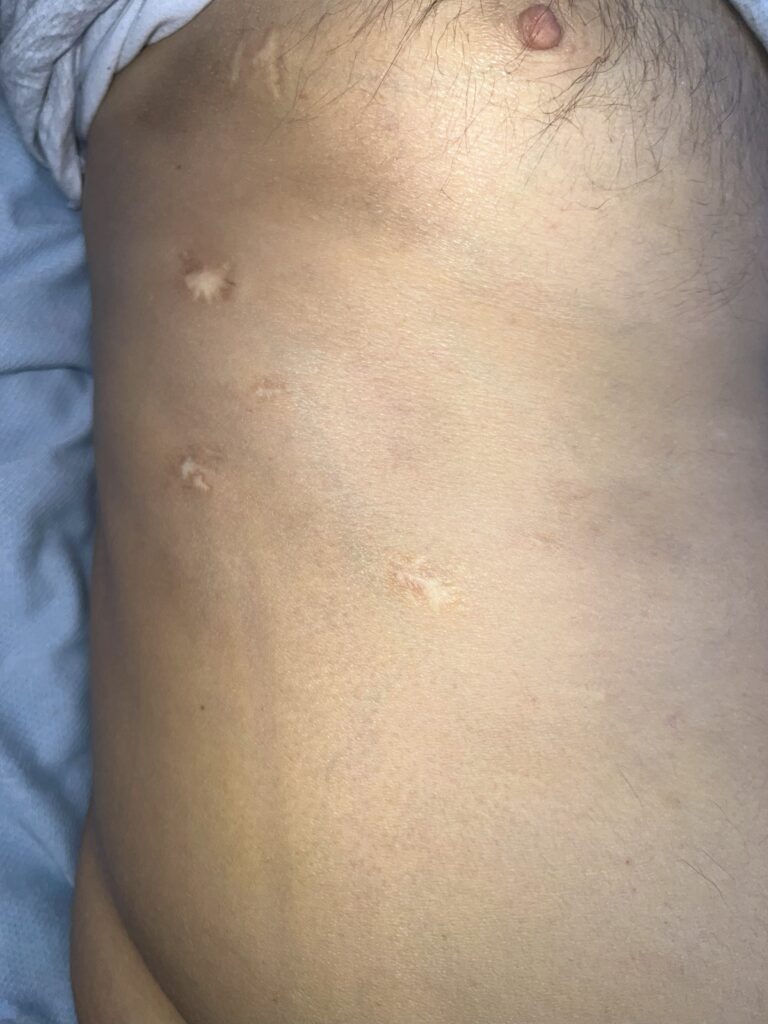
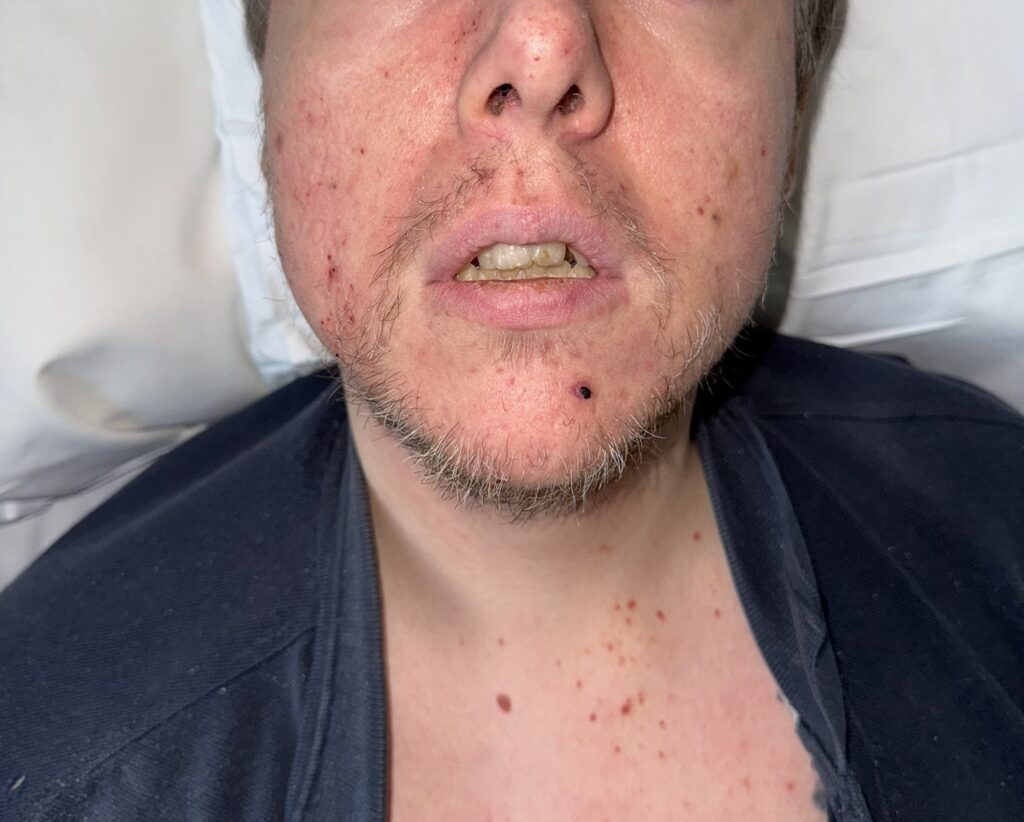
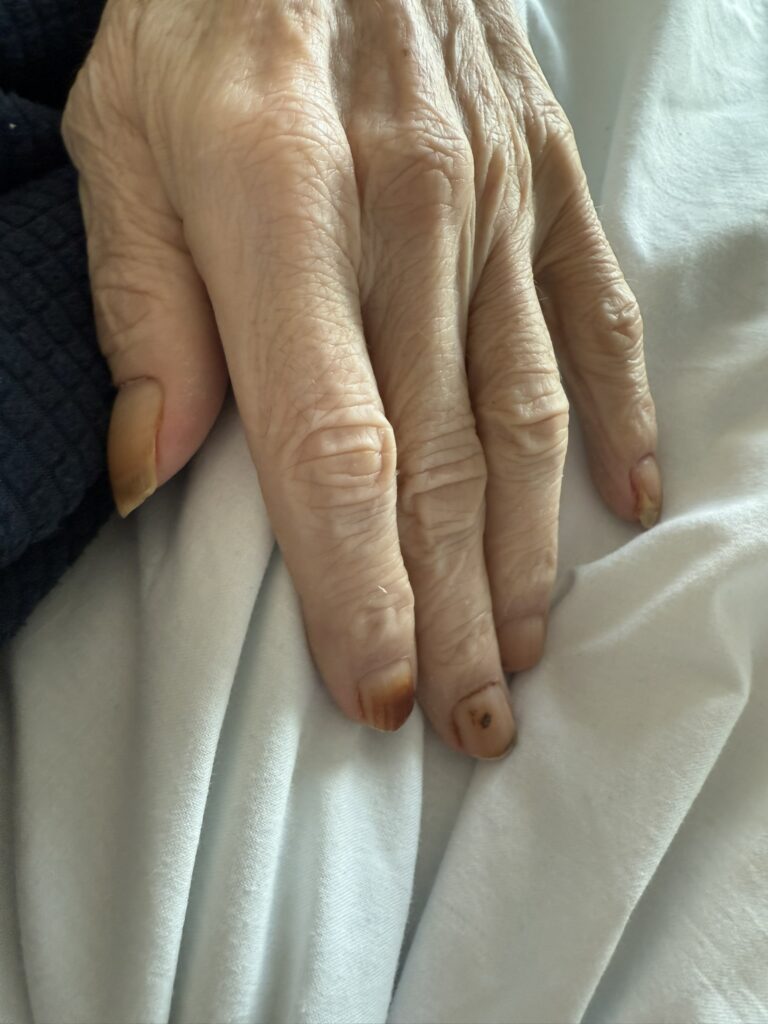
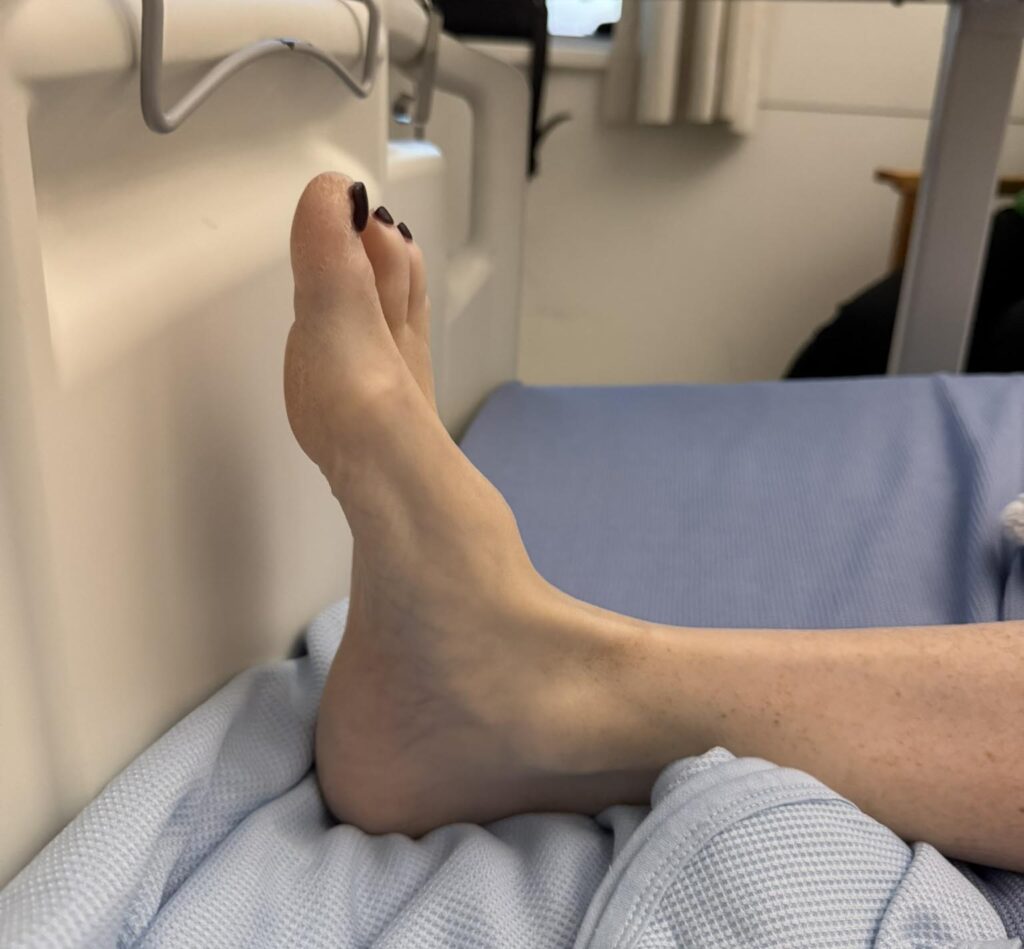
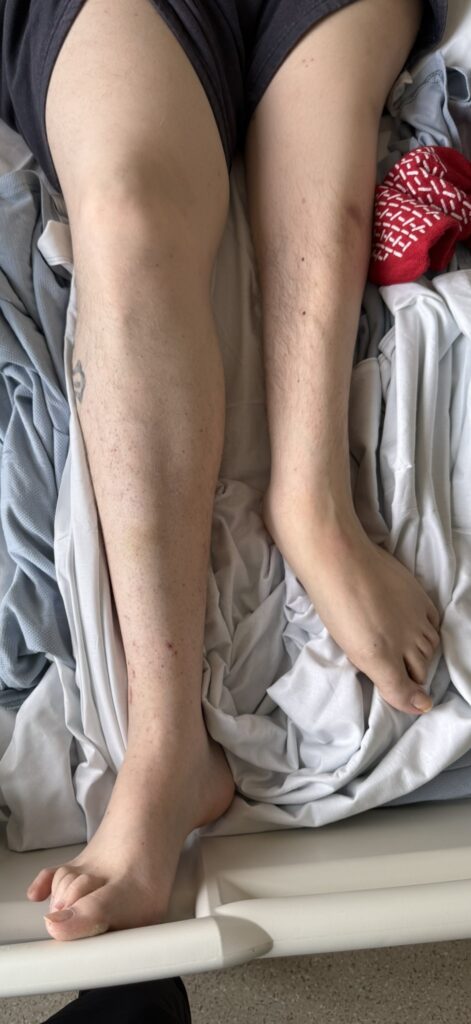
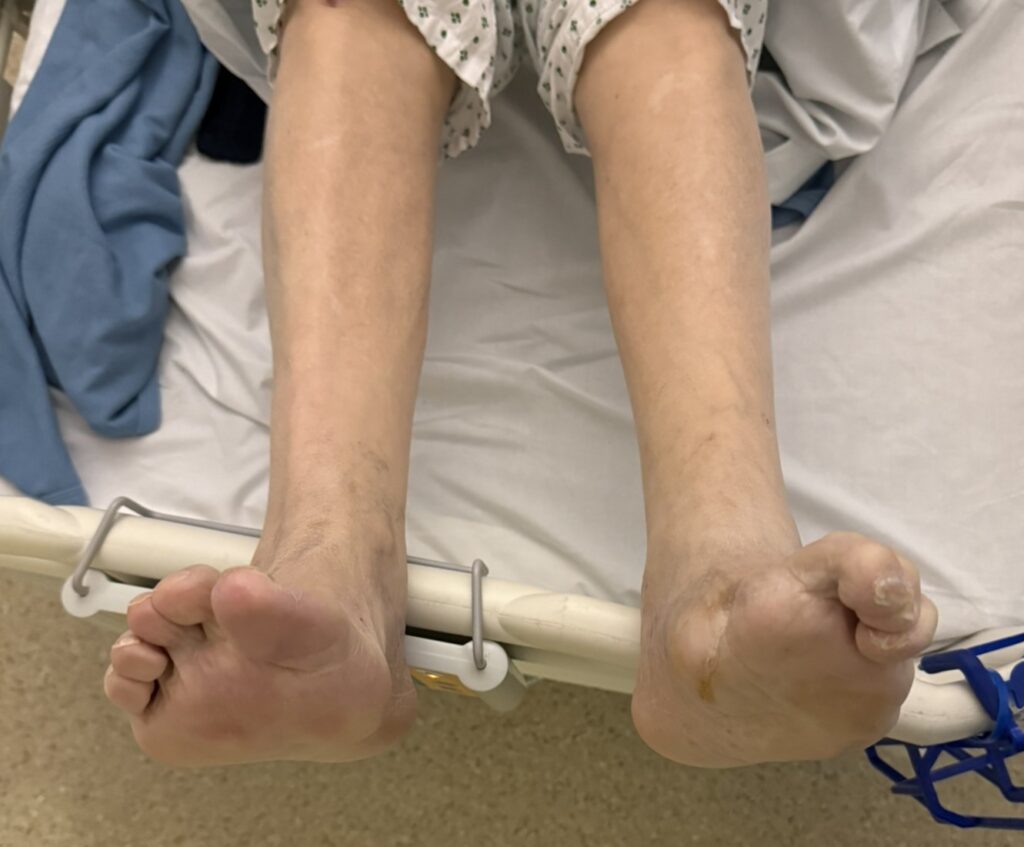
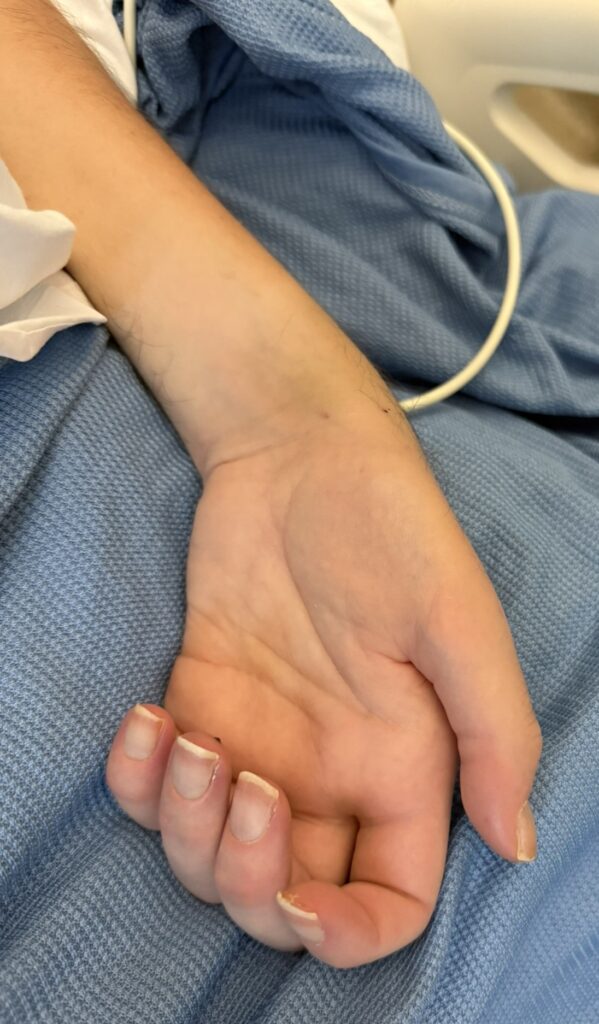
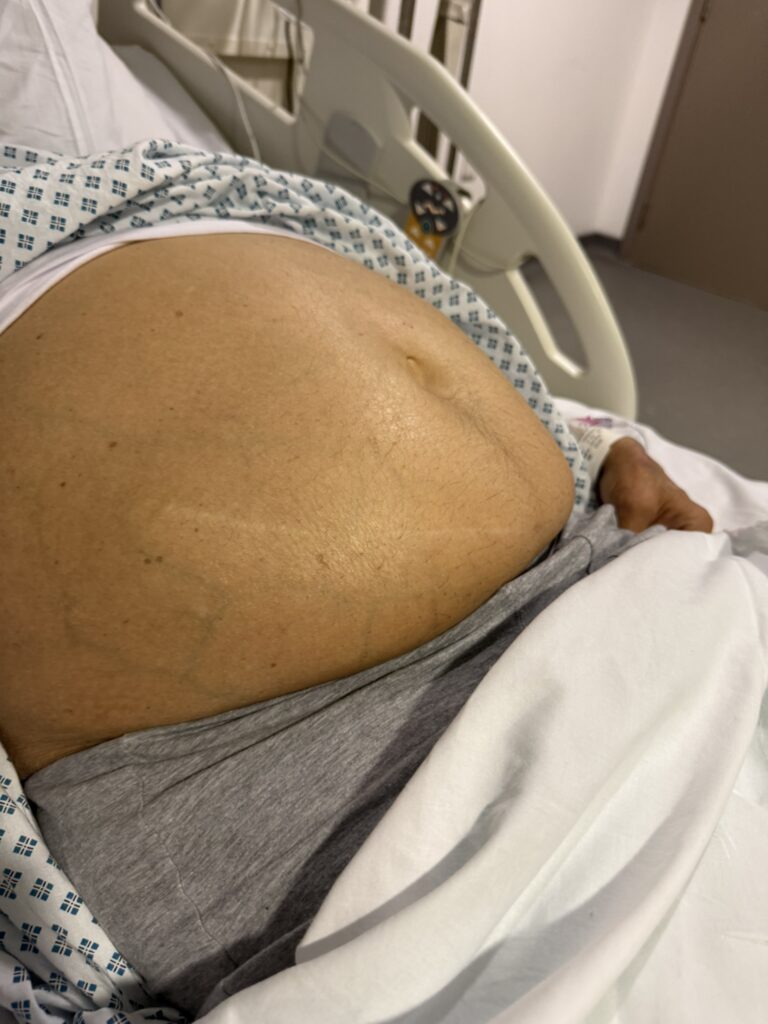
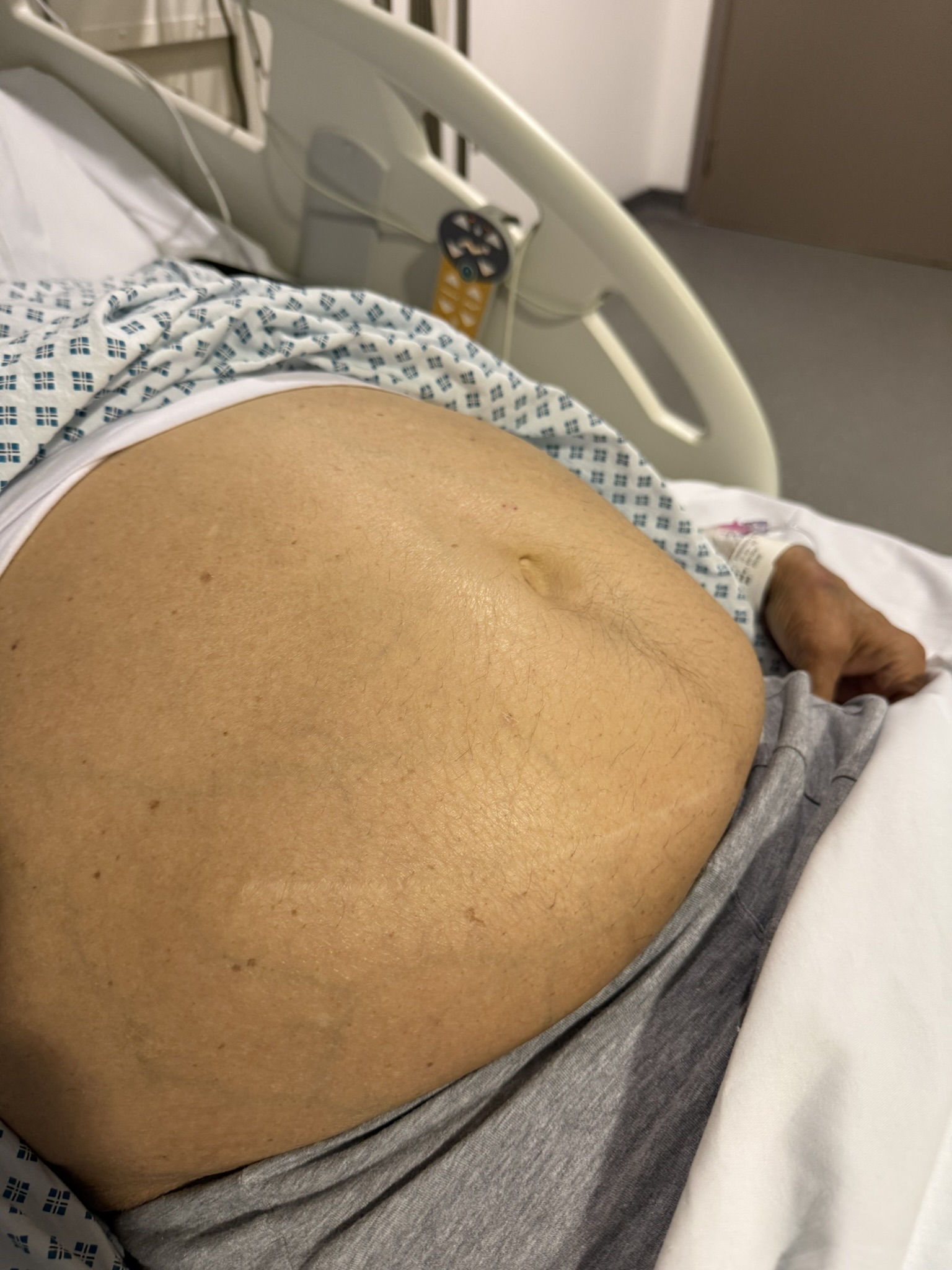
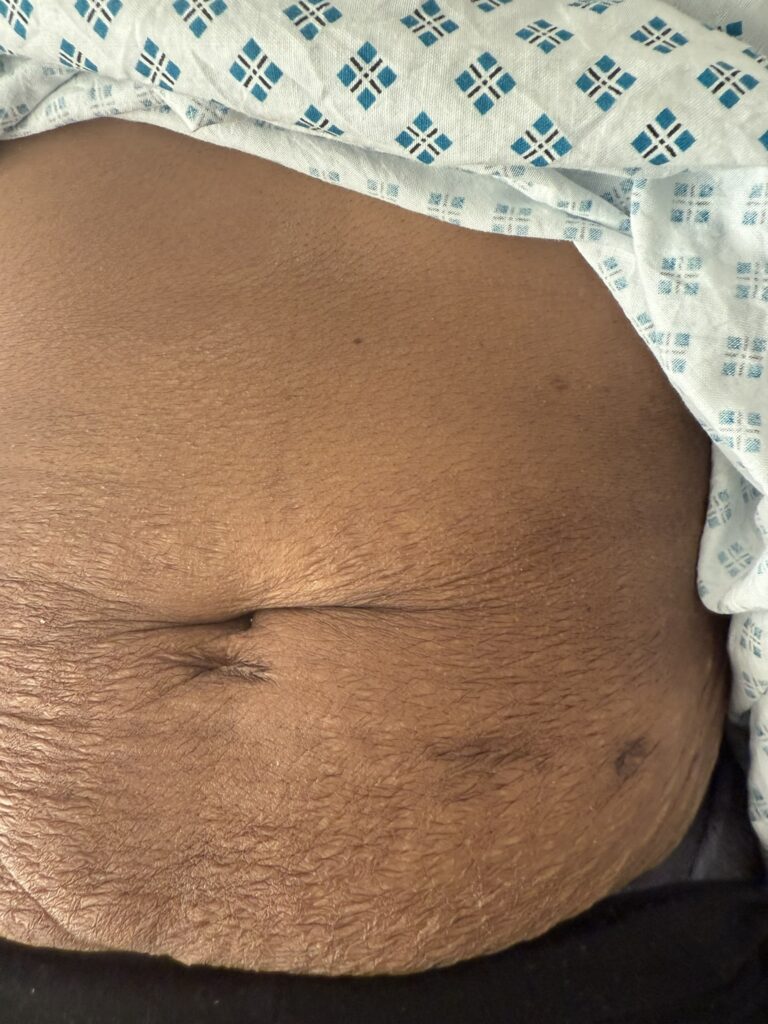
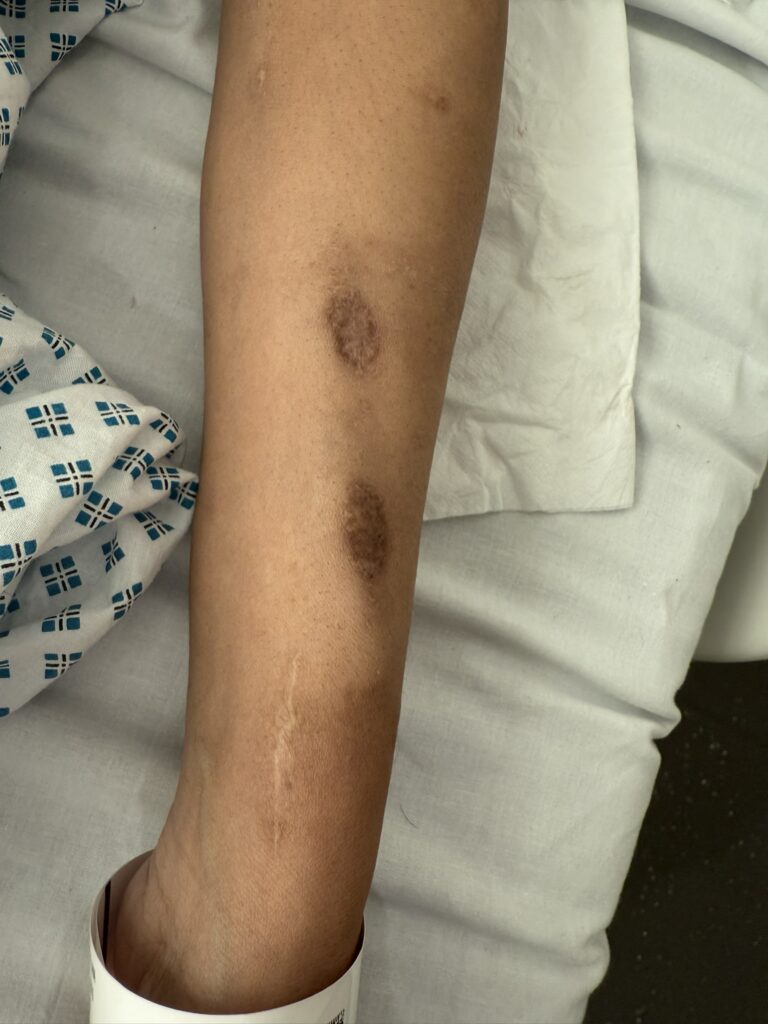
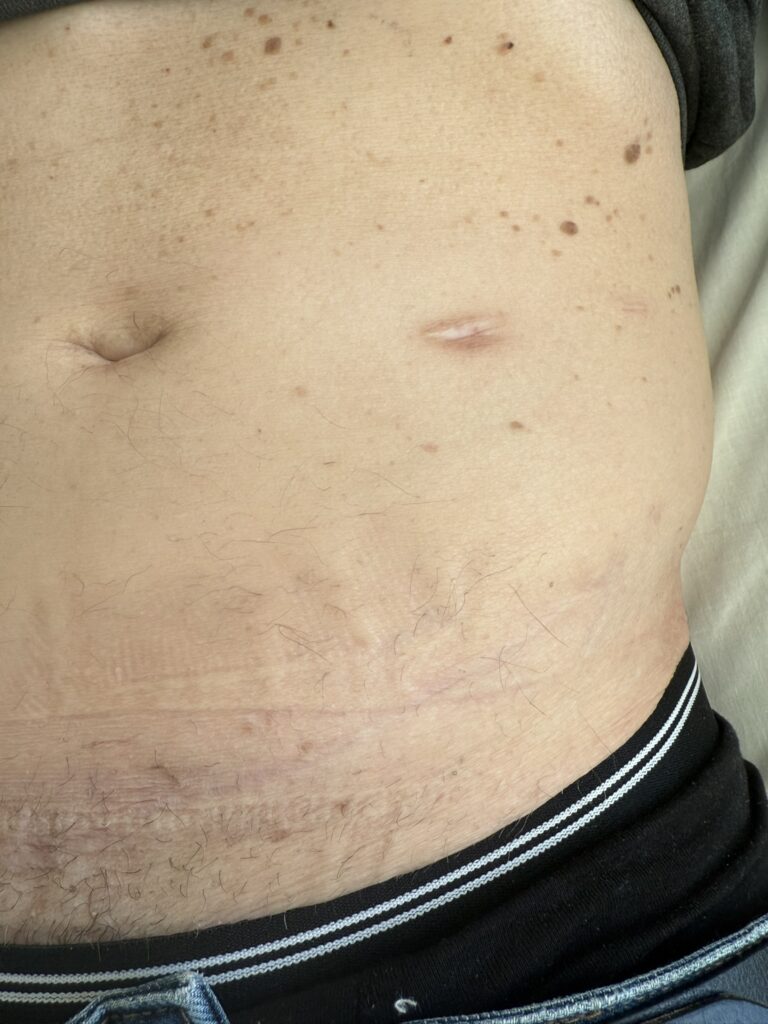
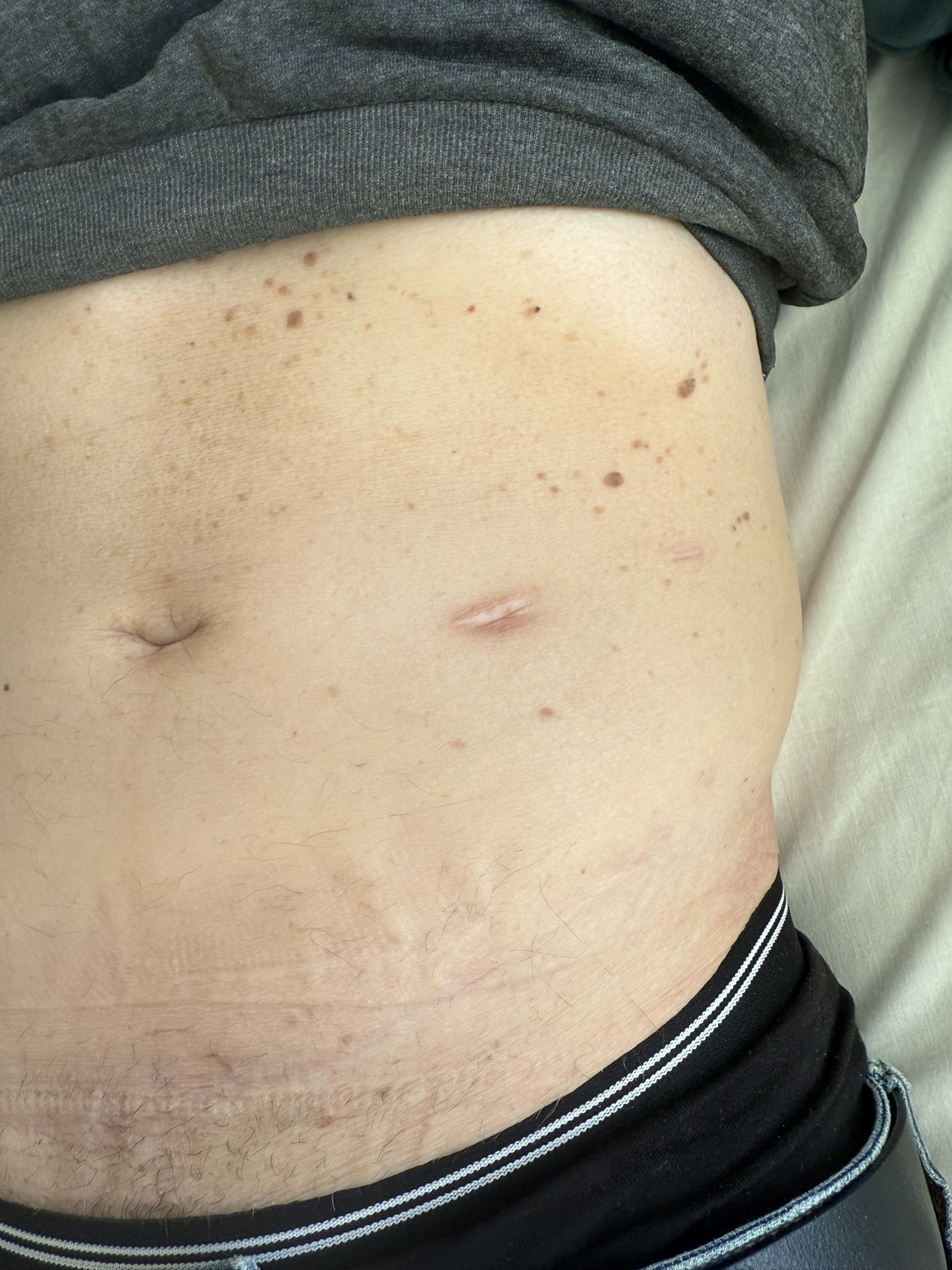
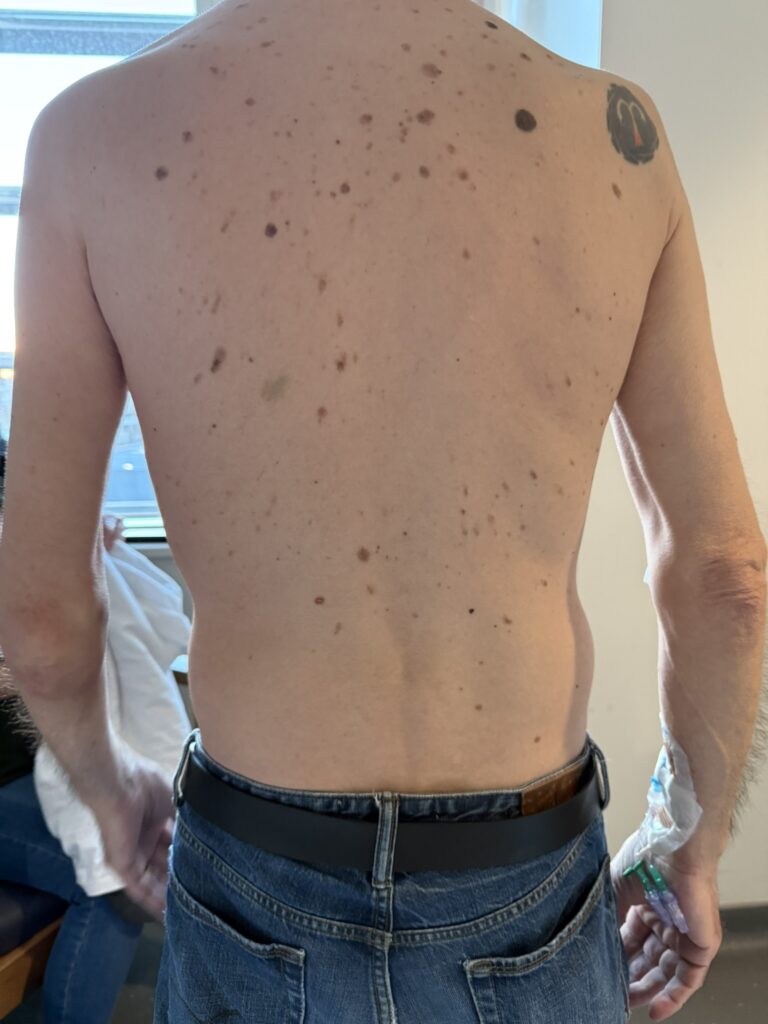
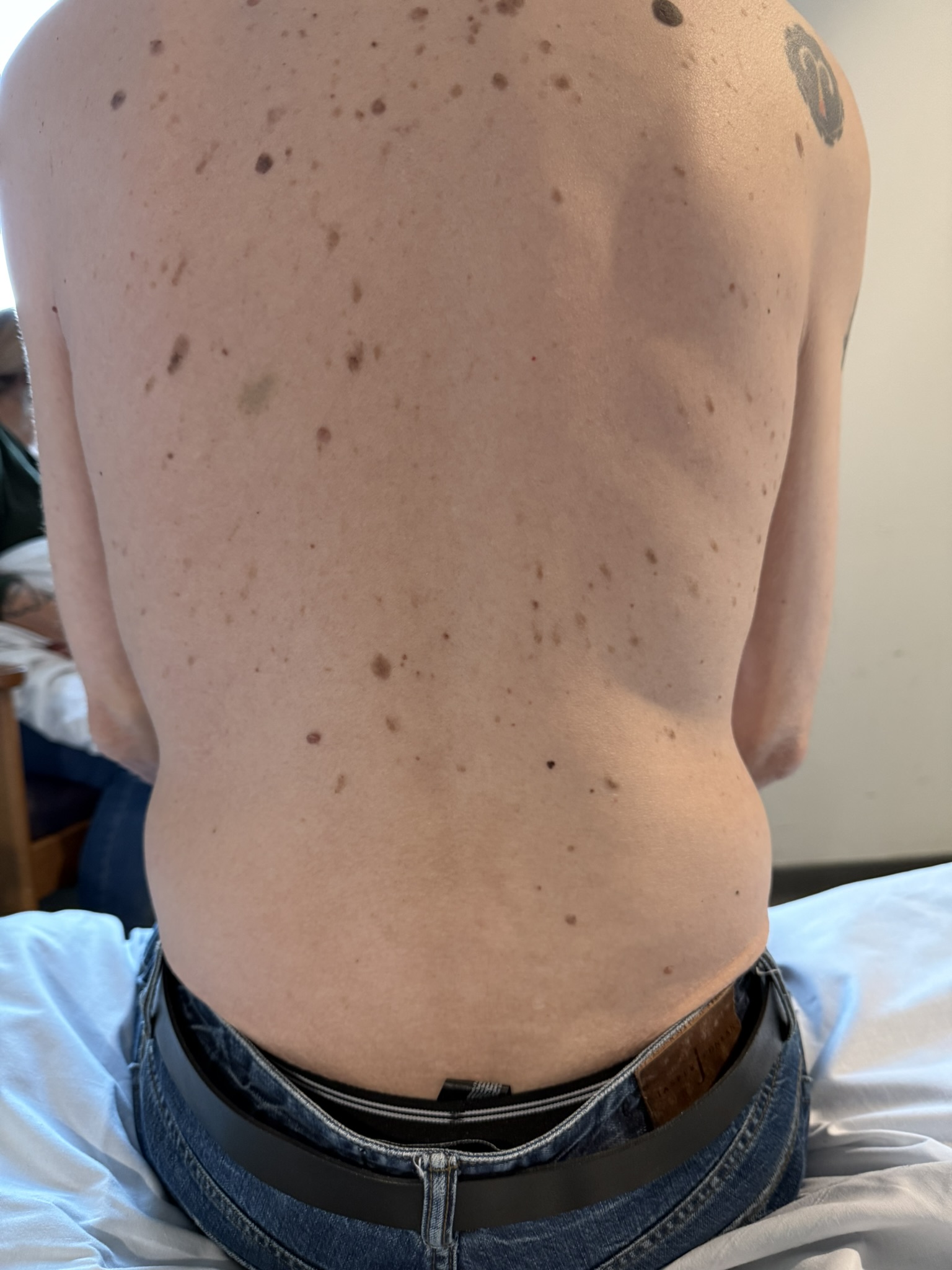
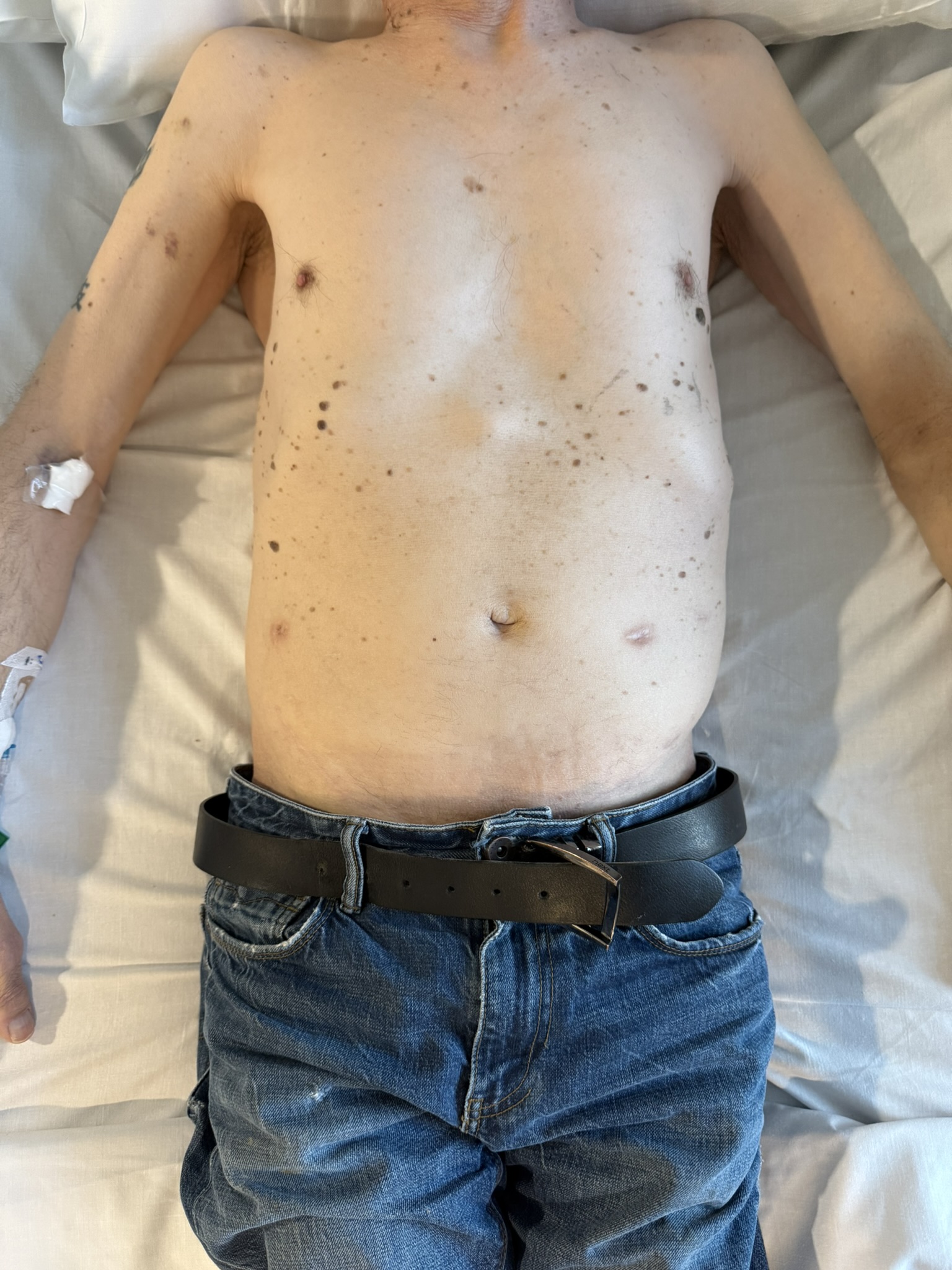
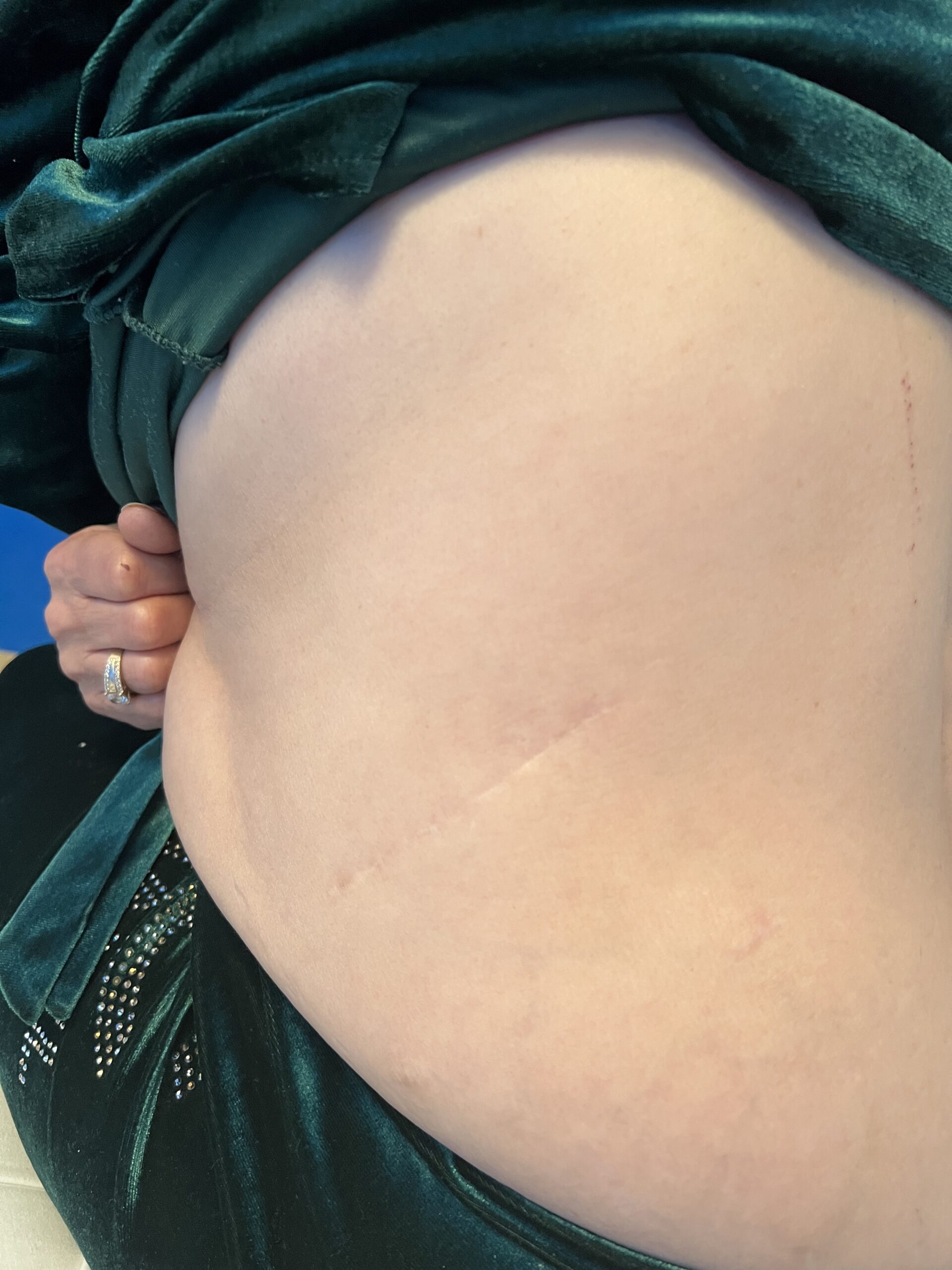
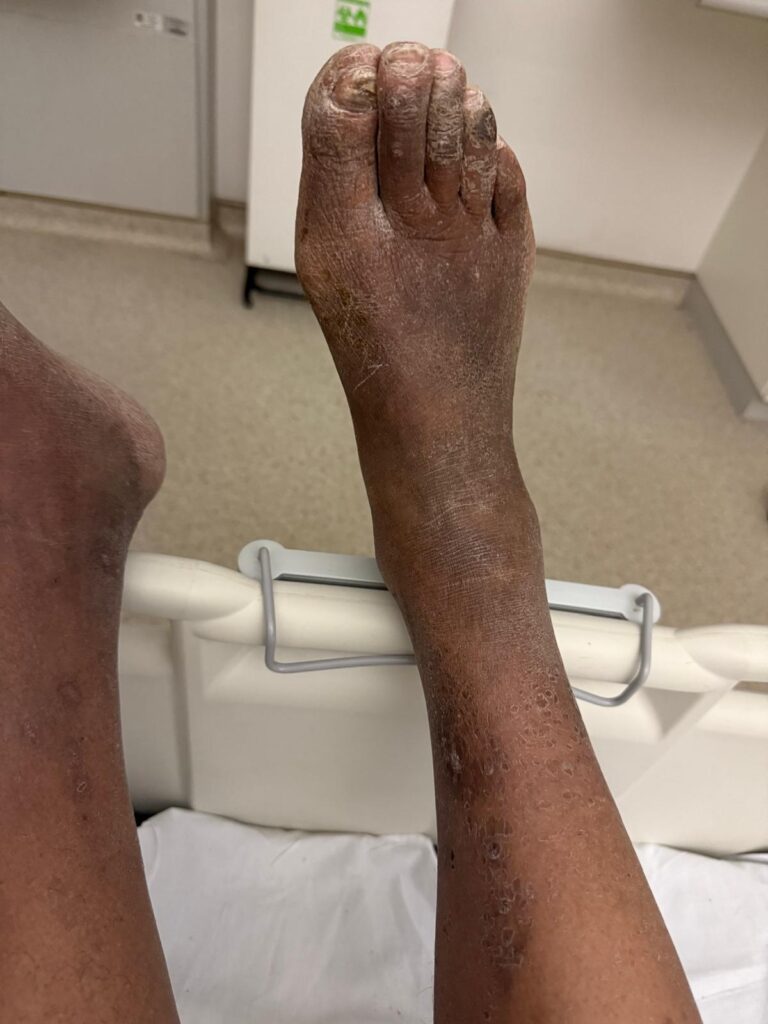
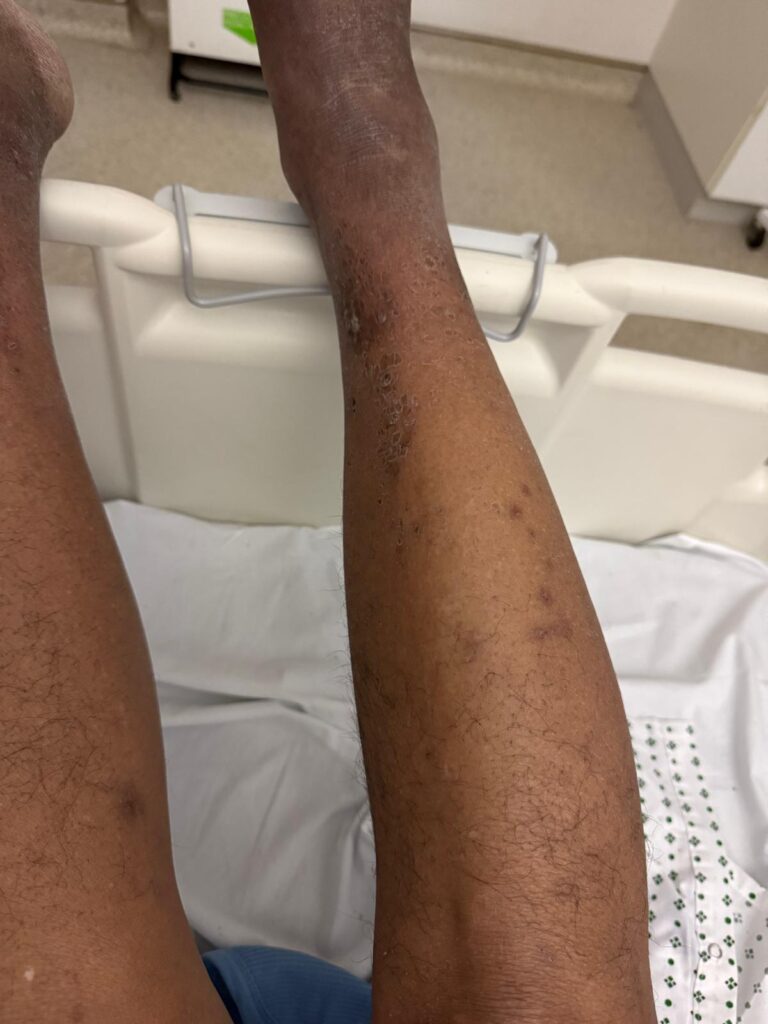
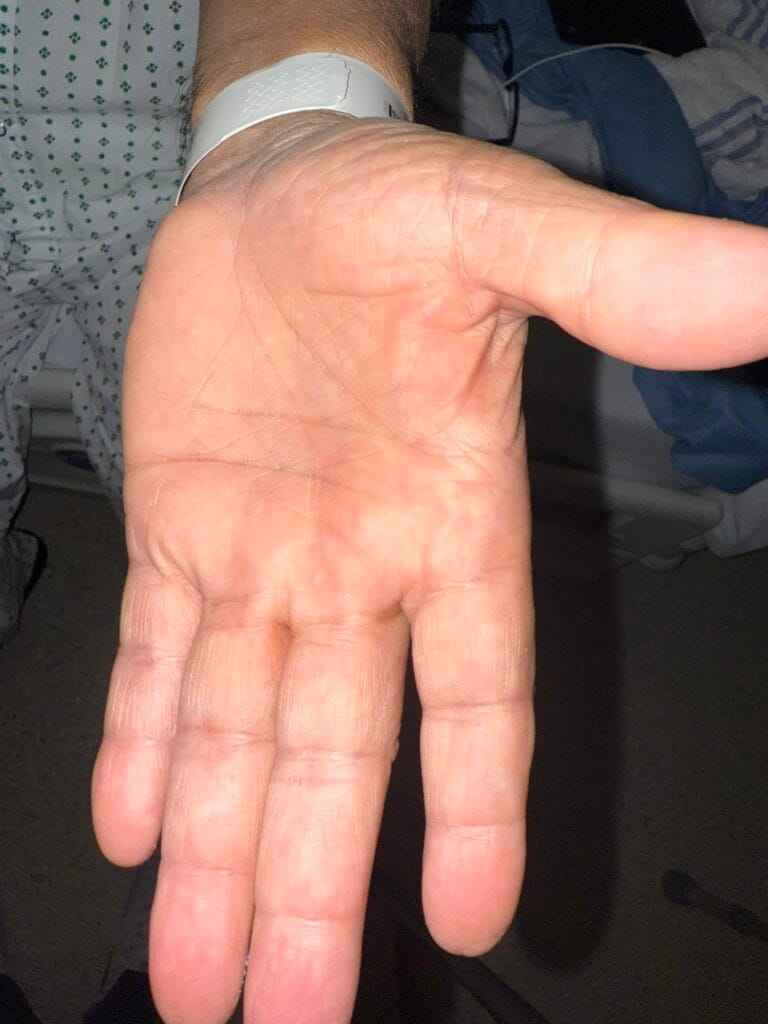
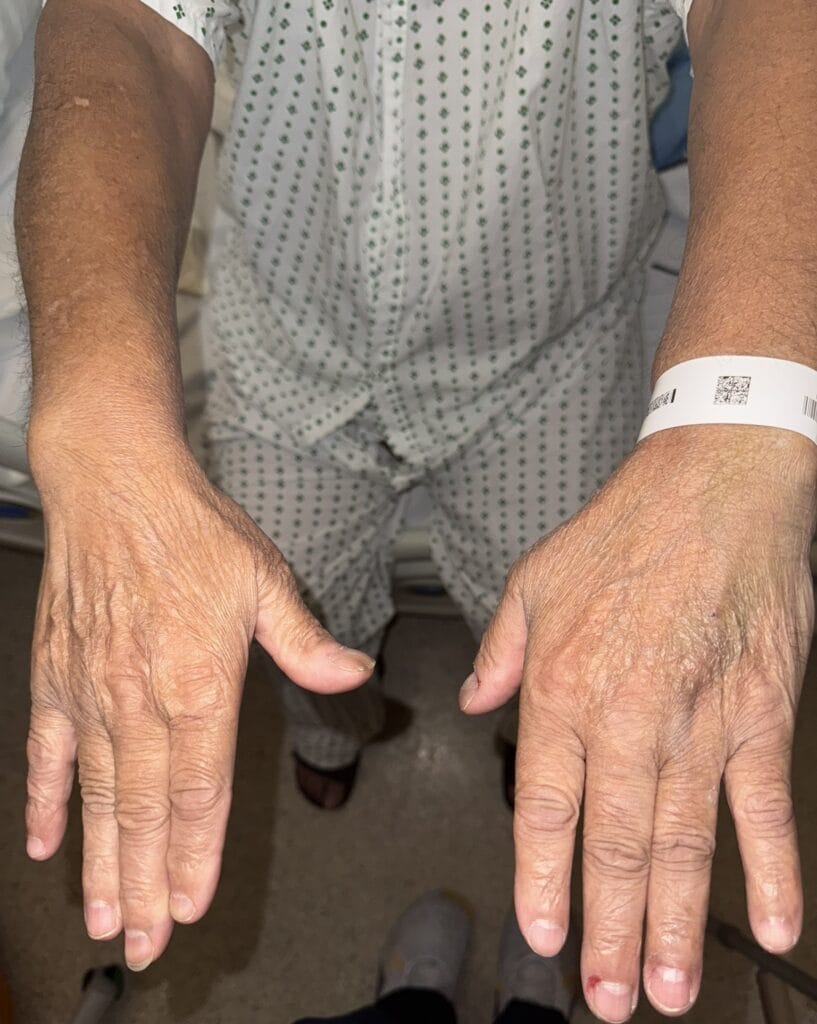
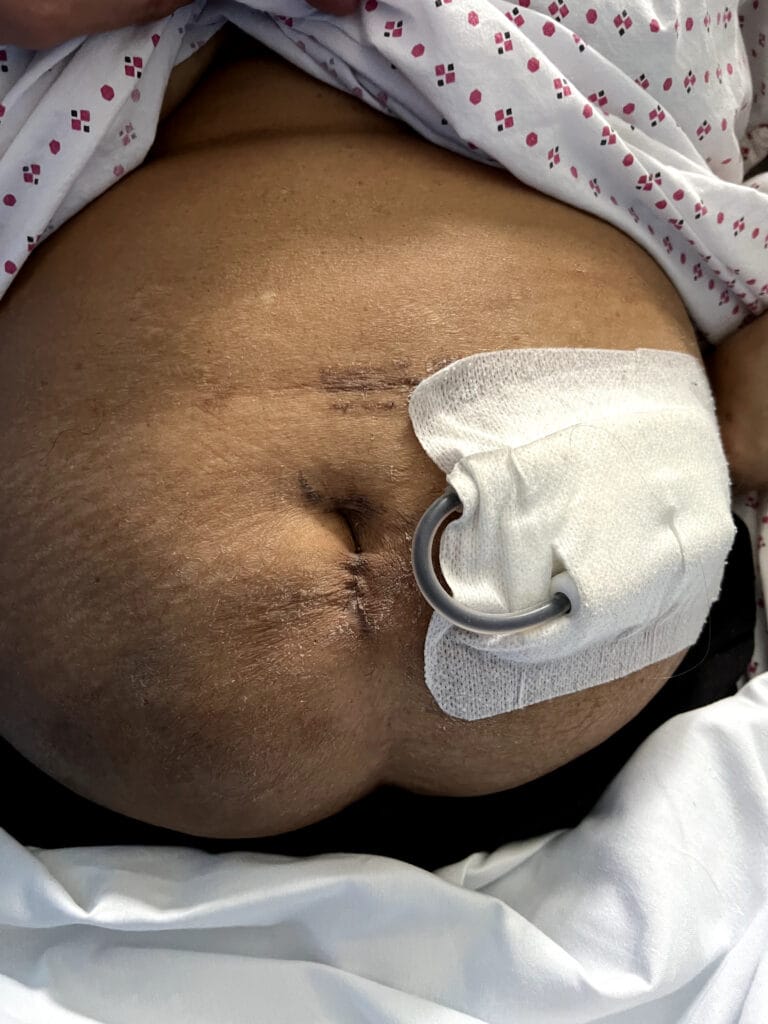
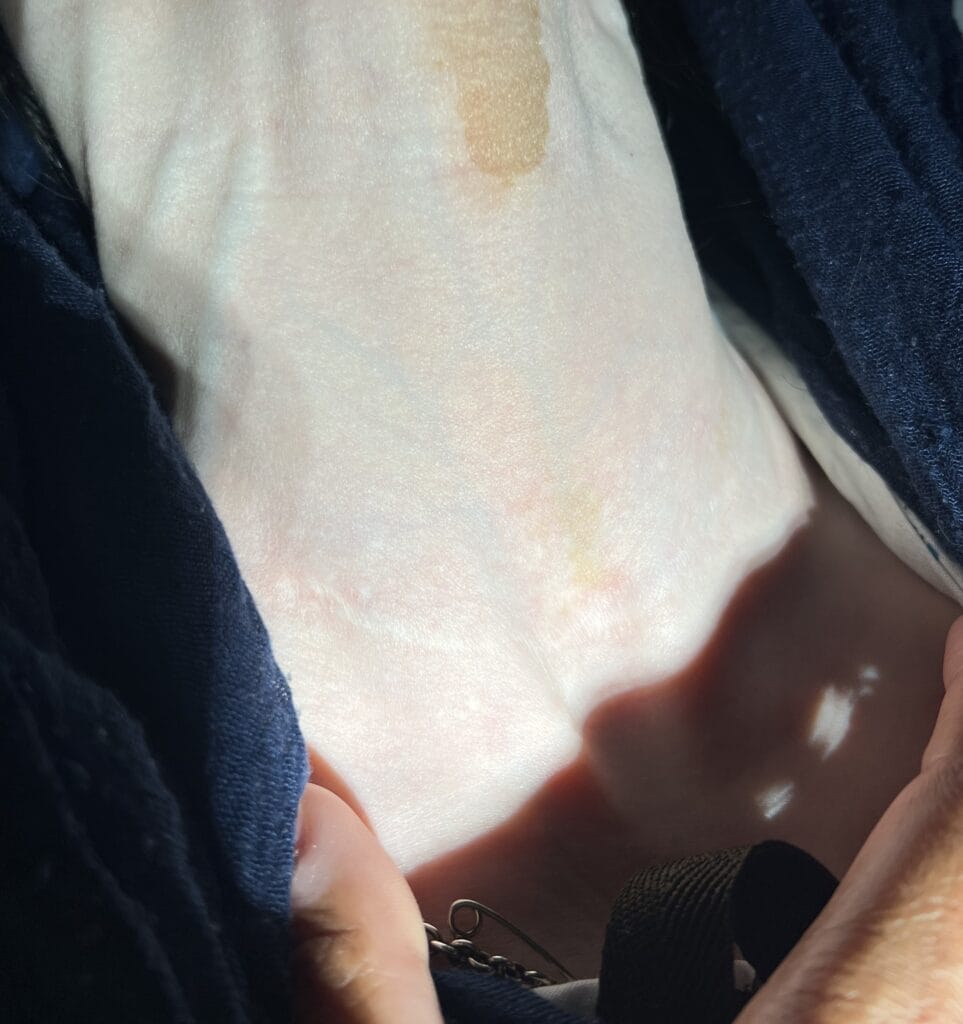
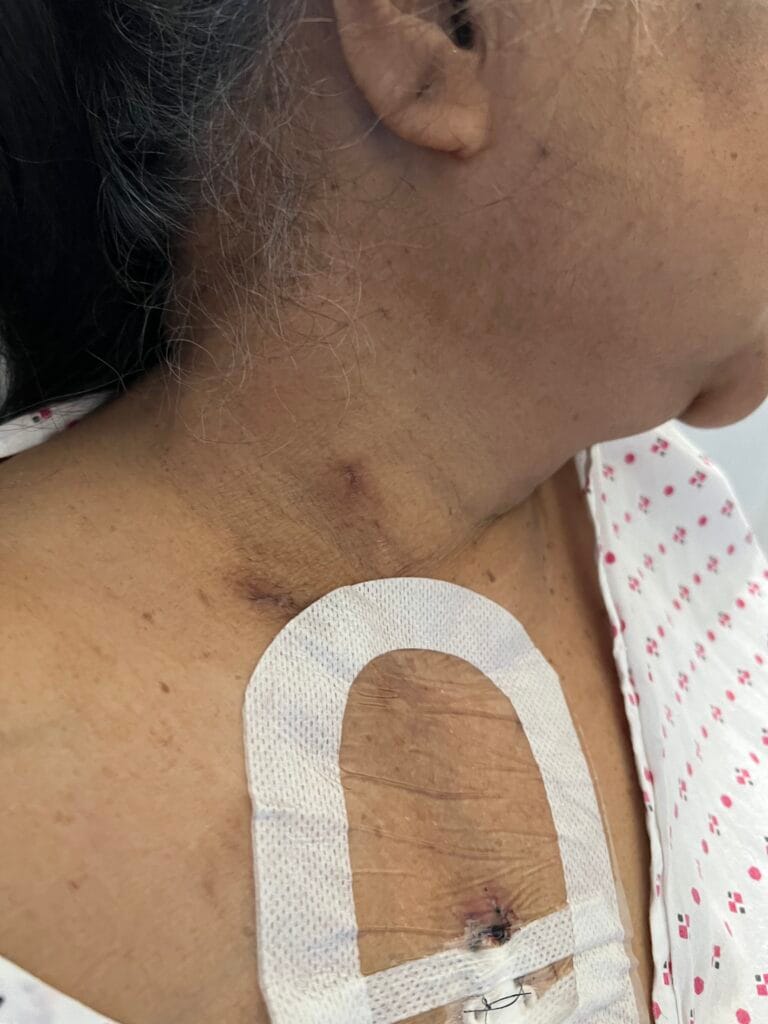
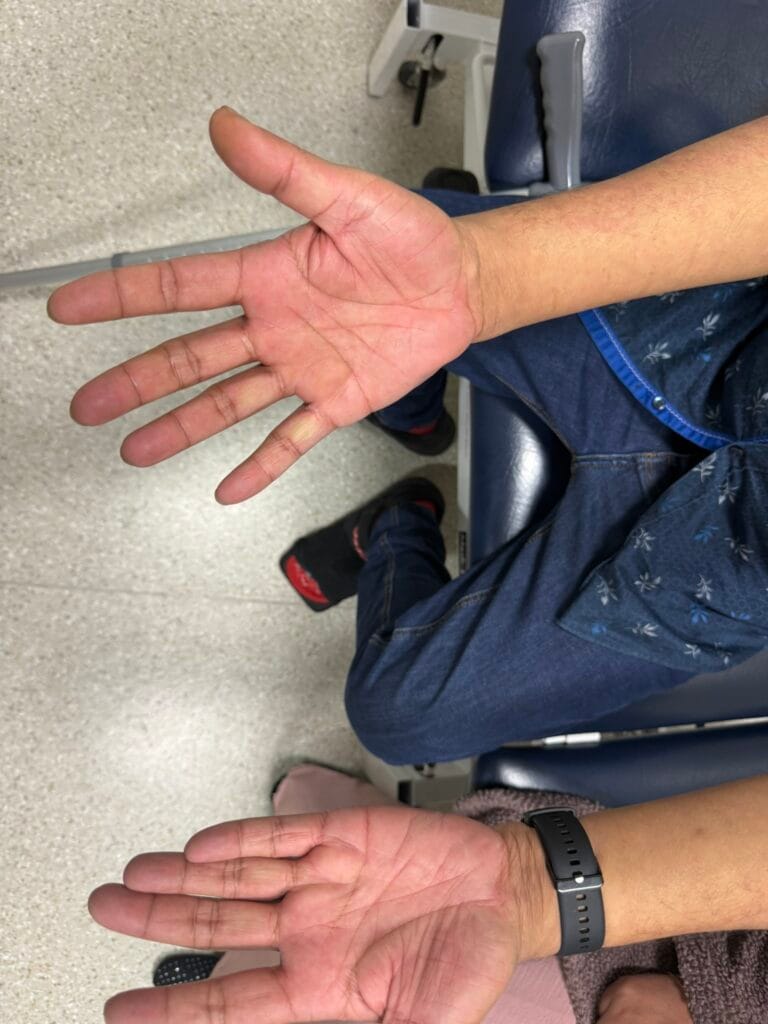
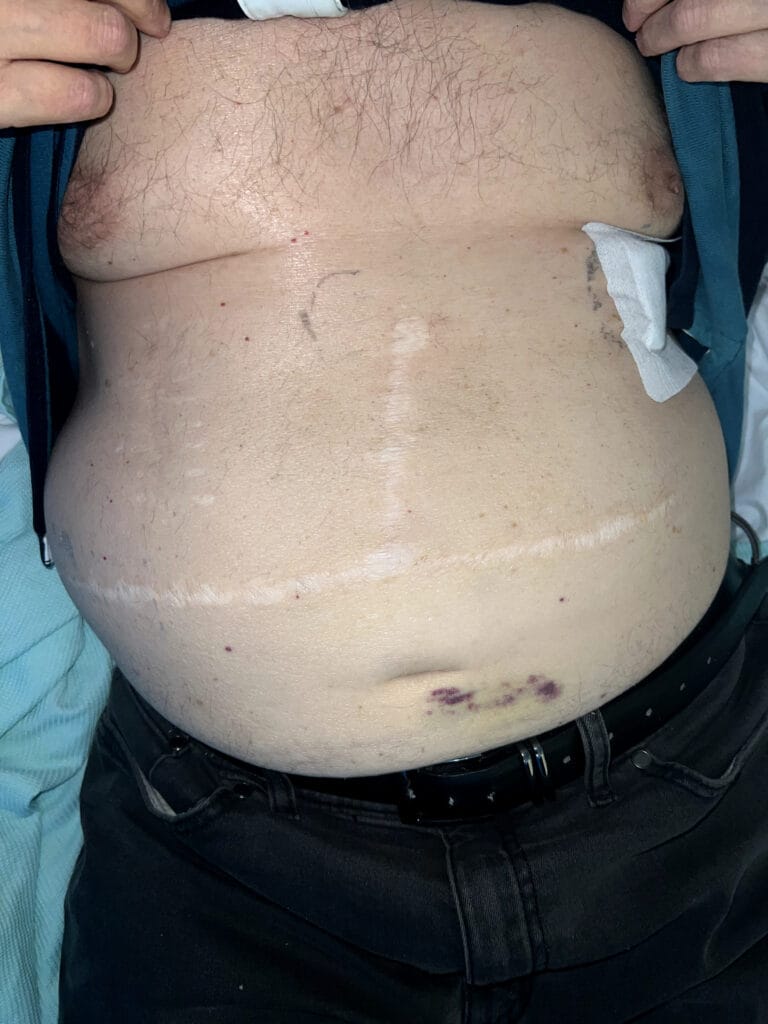
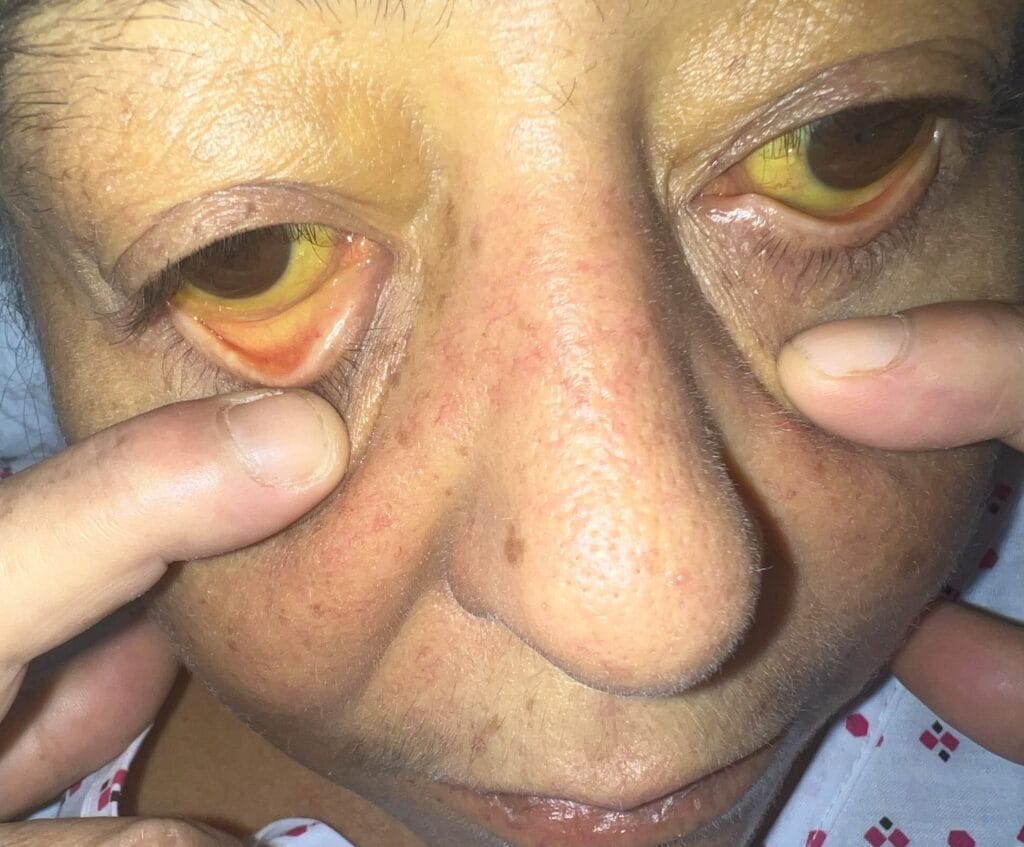
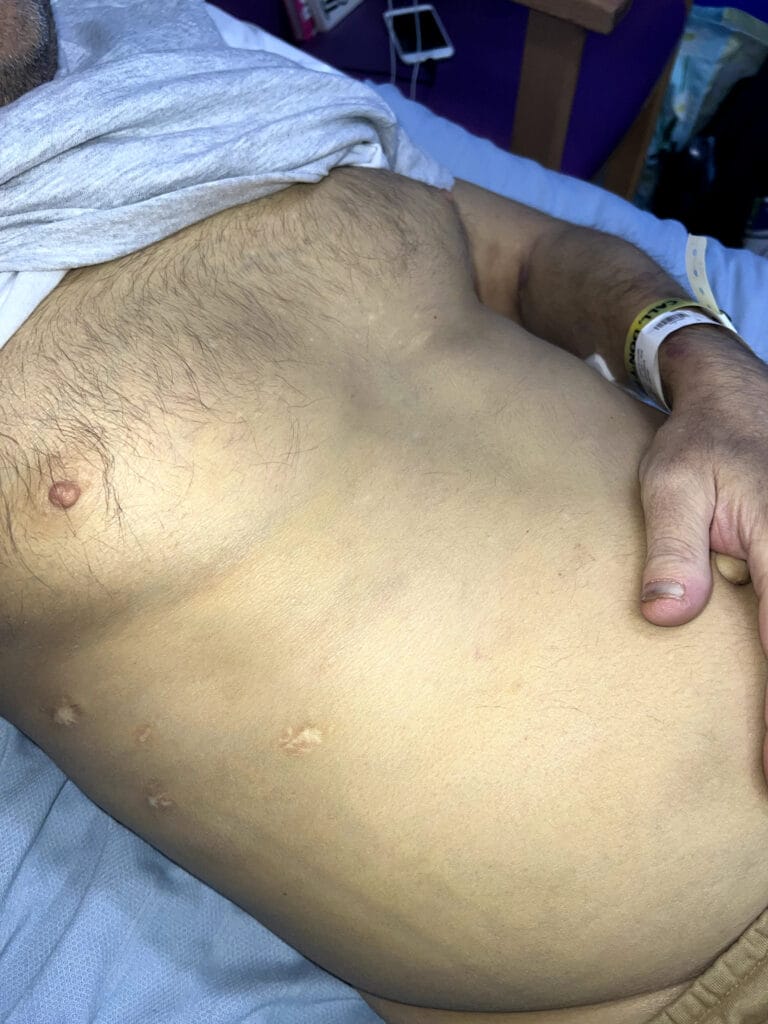
Neurofibromatosis is an autosomal dominant neurocutaneous disorder characterised by multiple cafe-au-lait spots, neurofibromas and variable involvement of the nervous system, eyes, bones and skin.
Station Instructions: Assess this patient presenting with multiple skin lesions.1. Key History‑Taking Points
Skin Lesions:
When first noticed? Increasing in number or size?
Any pain, itching, or disfigurement?
Any nodules under the skin (neurofibromas)?
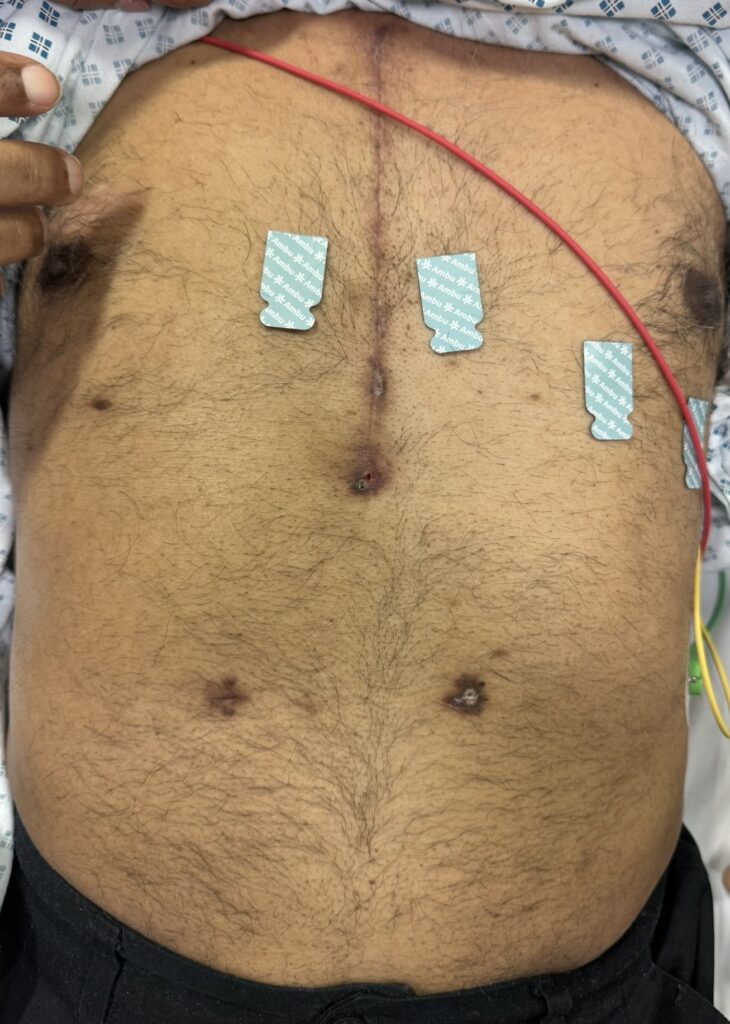
Café-au-lait macules: number, distribution, onset (>6 in Neurofibromatosis)
Axillary or inguinal freckling
Neurological Symptoms:
Headache, visual changes (optic glioma)
Hearing loss, tinnitus, balance disturbance (vestibular schwannoma in NF2)
Seizures, weakness, paraesthesia, neuropathic pain
Learning difficulties or attention problems (common in NF1)
Musculoskeletal:
Scoliosis, bone deformities (bowed tibia, pseudoarthrosis)
Fracture history
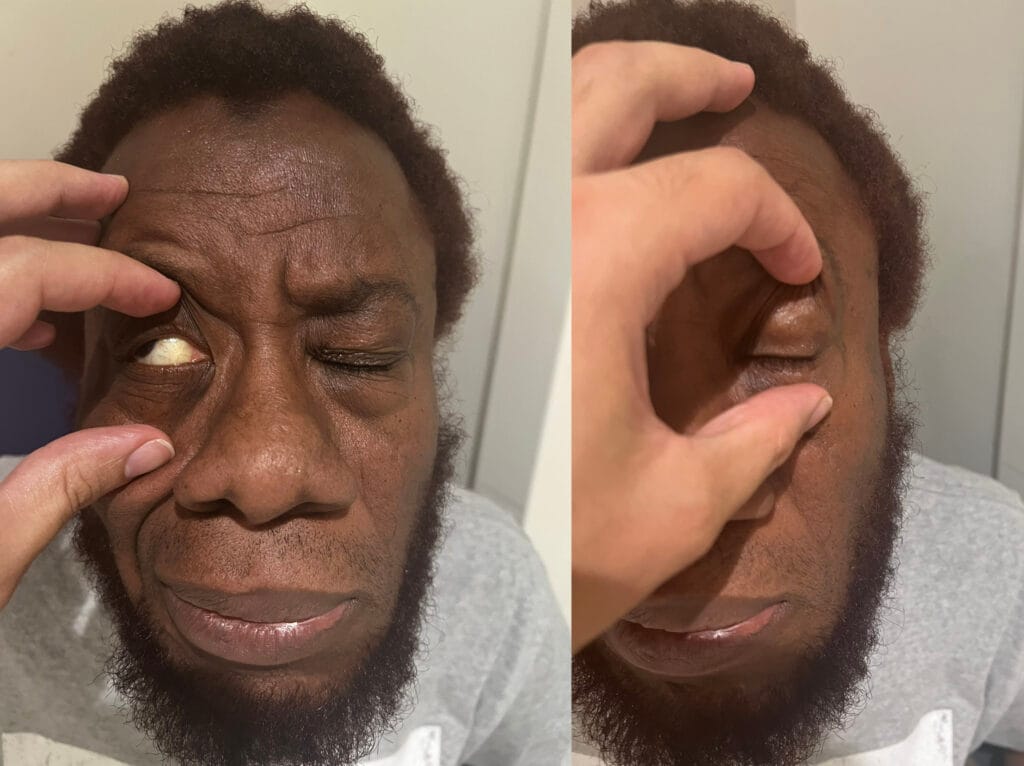
Ophthalmic:
Vision loss, double vision, proptosis, eye pain
Lisch nodules or optic glioma symptoms
Family History:
Any relatives diagnosed with NF1/NF2 or unexplained skin lesions, deafness, or early blindness
Mode of inheritance (autosomal dominant)
Functional Impact:
Cosmetic concerns, psychological distress, functional disability
2. Key Examination Findings
General Appearance:
Multiple café-au-lait macules (>6, >5 mm in prepubertal or >15 mm in adults)
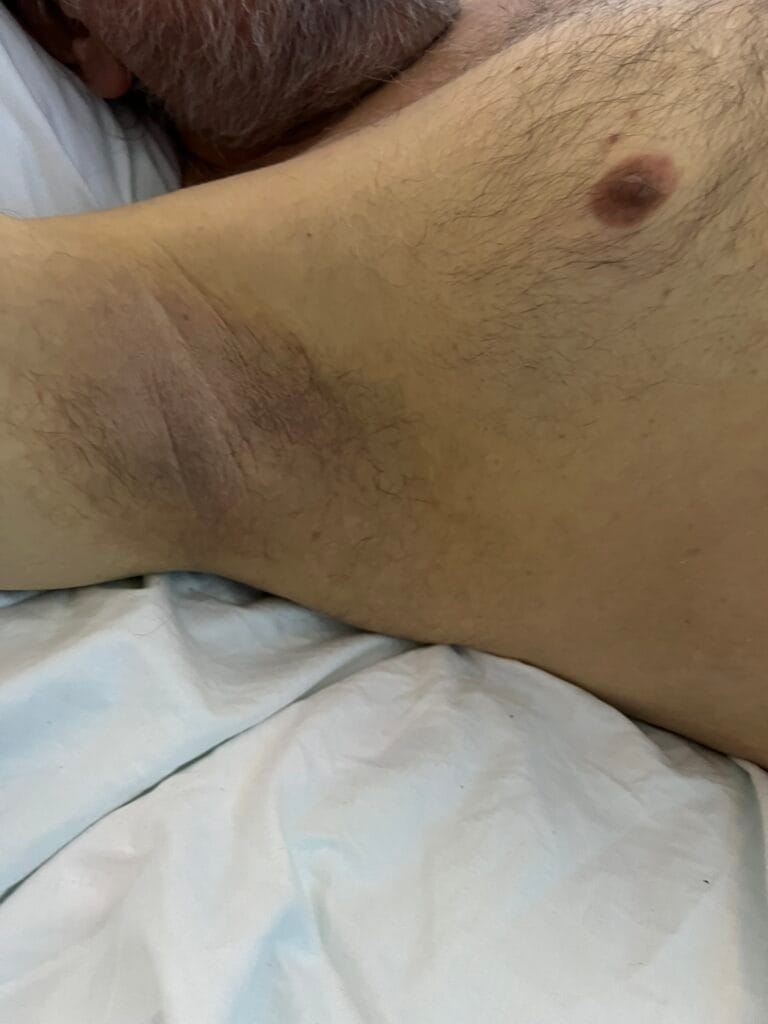
Axillary or inguinal freckling (Crowe sign)
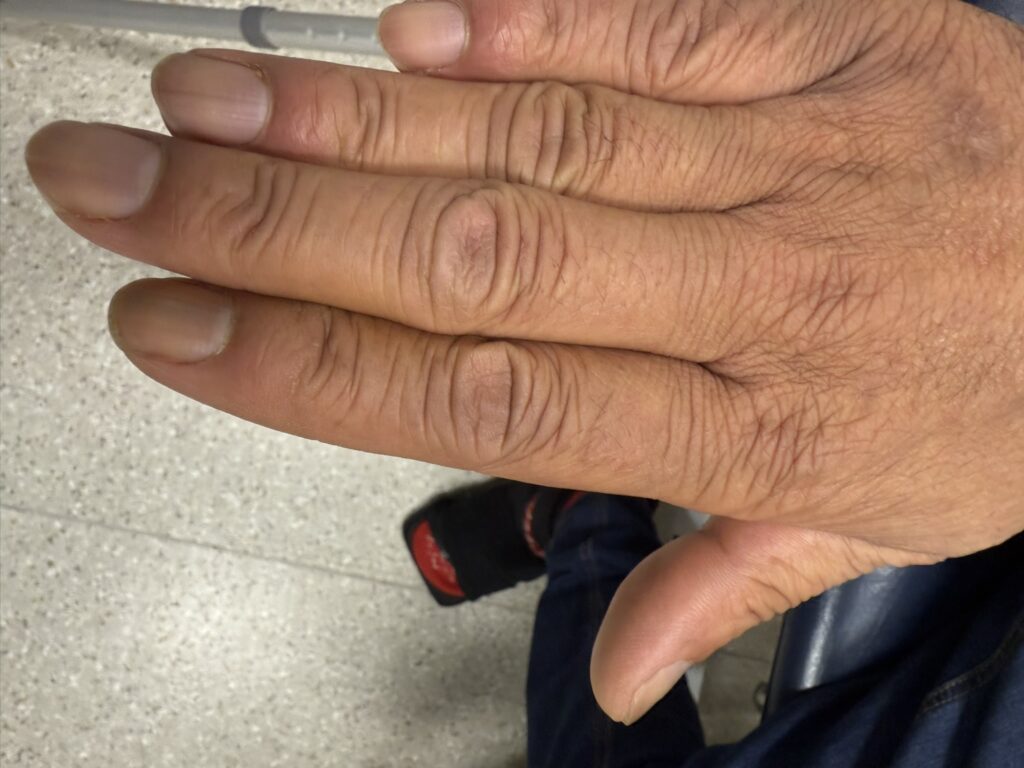
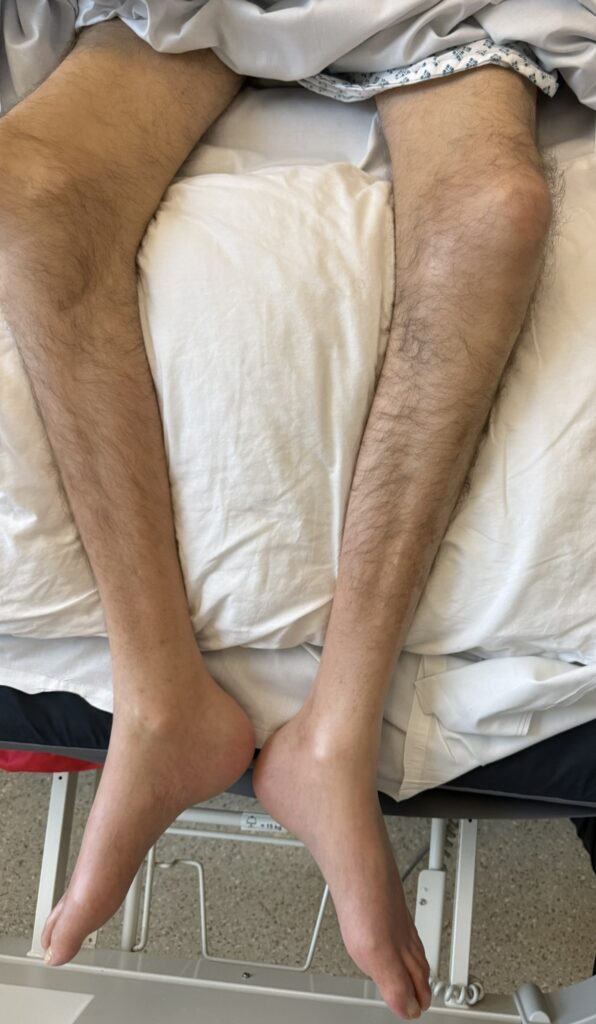
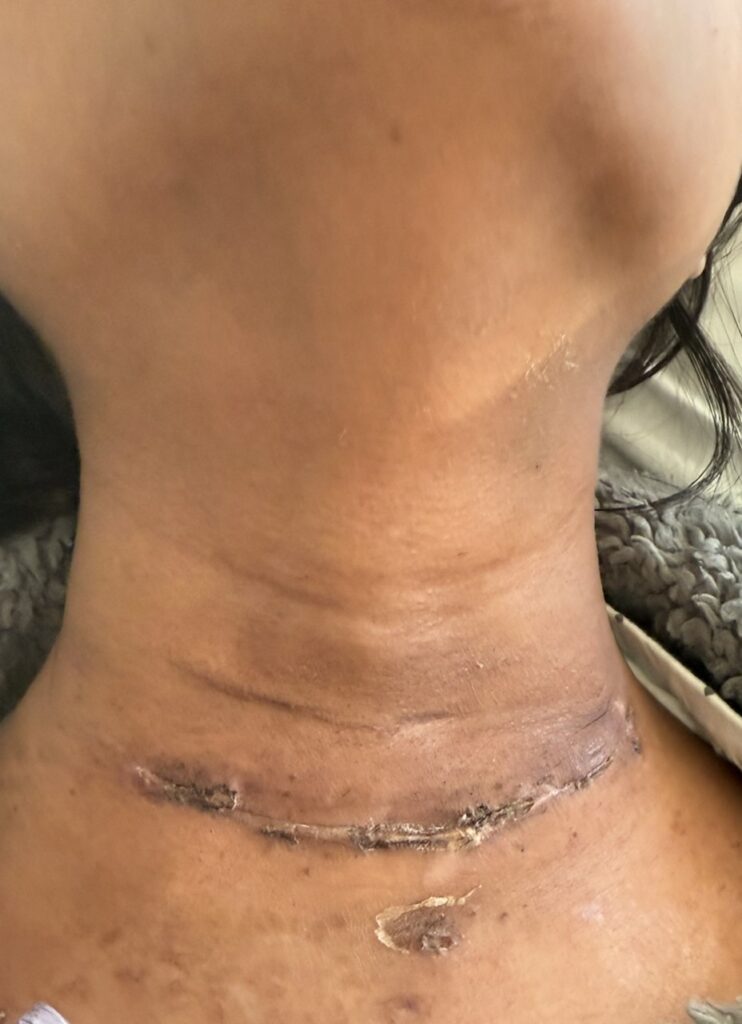
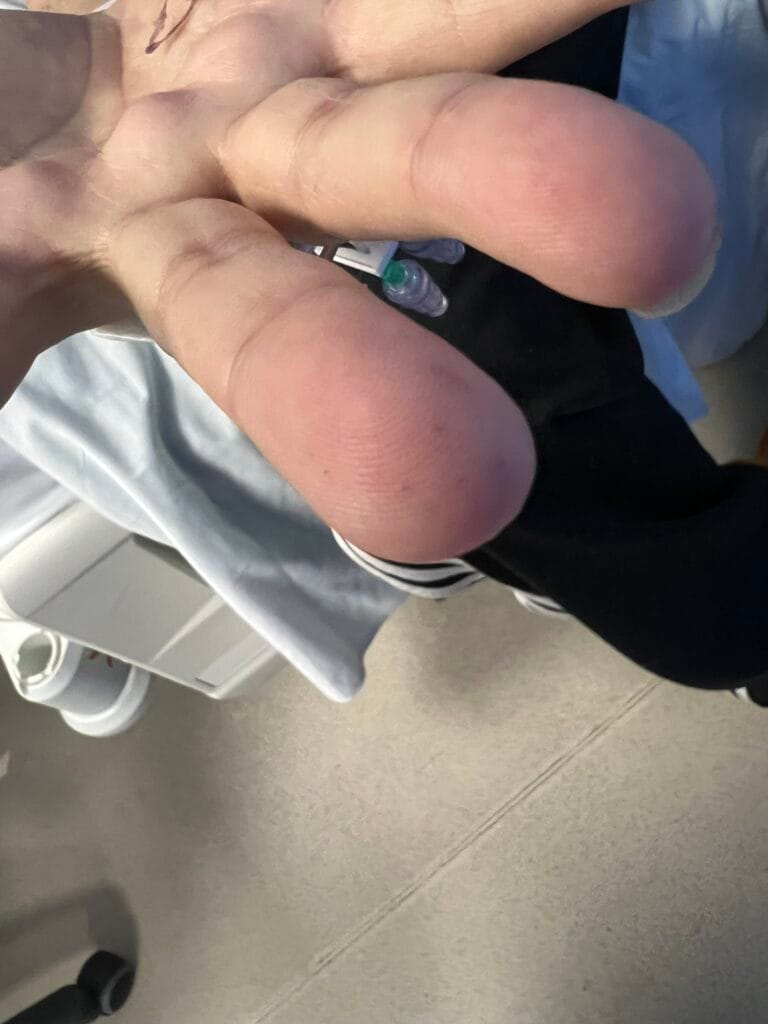
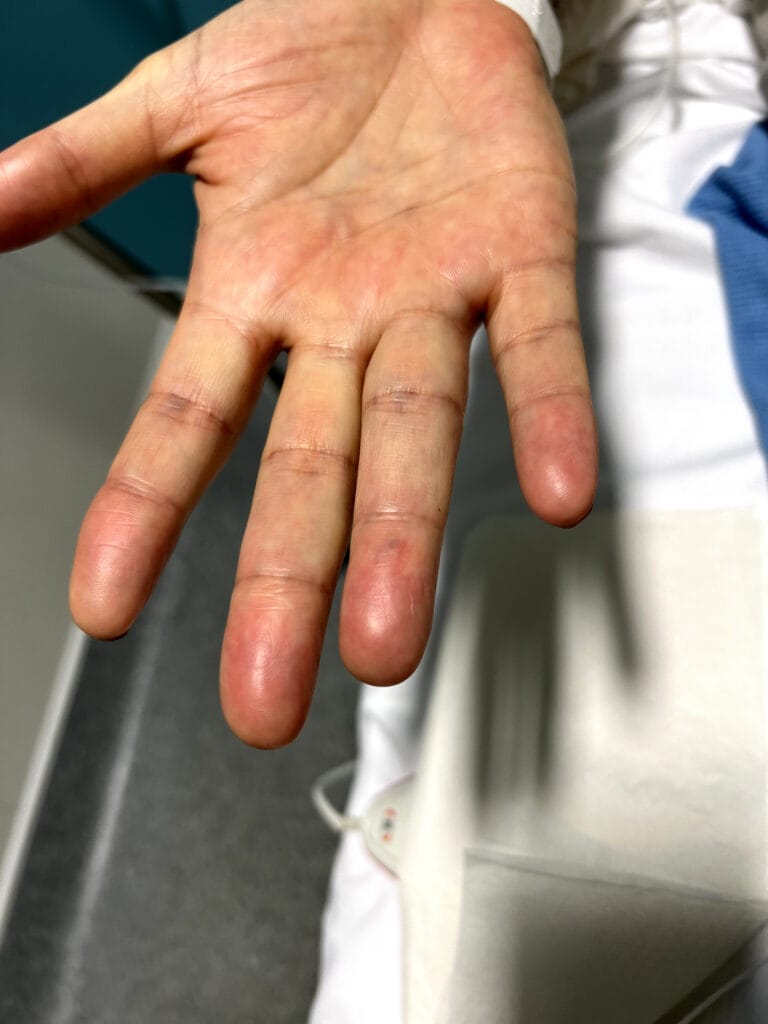
Cutaneous neurofibromas: soft, pedunculated lesions
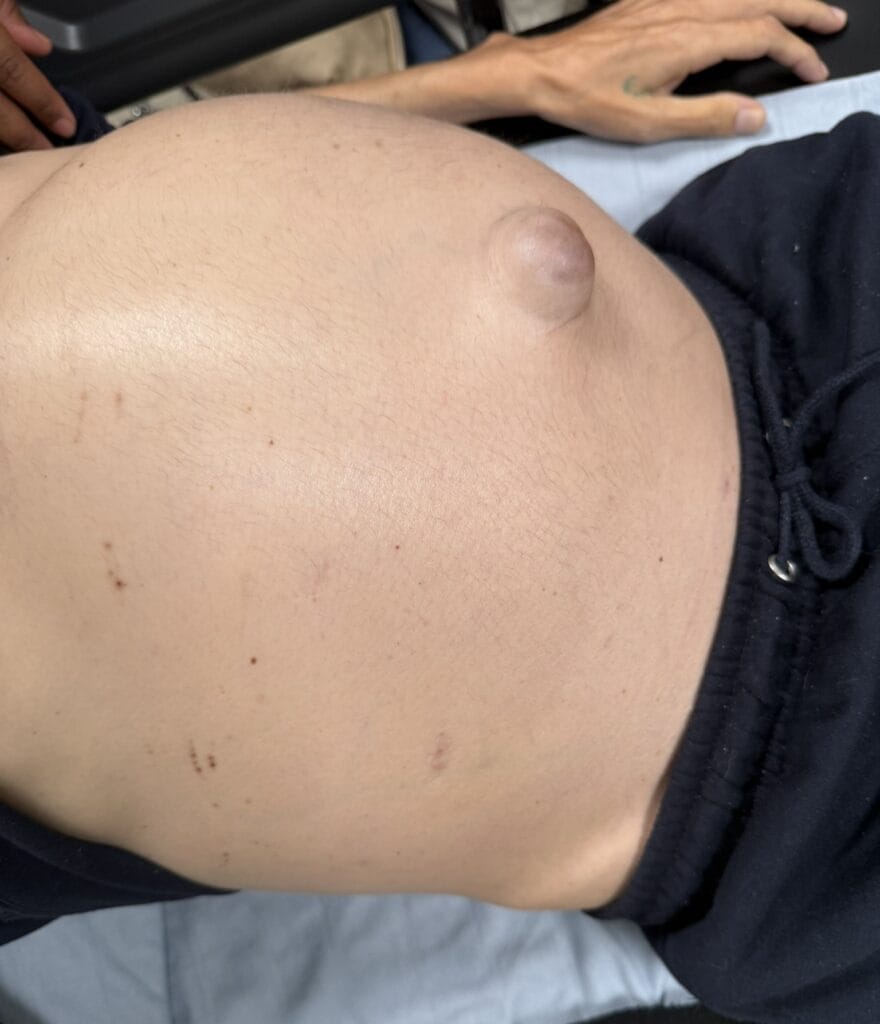
Plexiform neurofibromas: large, nodular, may cause disfigurement
Ophtalmological:
Lisch nodules (iris hamartomas) — slit lamp exam
Proptosis or visual loss (optic glioma)
Neurological:
Cranial nerve deficits (esp. CN VIII in NF2)
Peripheral neuropathy
Weakness, spasticity, gait disturbance
Musculoskeletal:
Scoliosis
Limb asymmetry
Pseudoarthrosis or tibial bowing
3. Specific Investigations
Laboratory & Genetic Testing:
Clinical diagnosis based on NIH criteria
Genetic testing for NF1 or NF2 mutations (if uncertain or for family counselling)
Imaging:
MRI Brain & Spine: to detect optic glioma, vestibular schwannomas, meningiomas, or spinal tumours
MRI Orbit: if visual symptoms present
Skeletal X-ray/MRI: for bone dysplasia, pseudoarthrosis, scoliosis
Ophthalmology:
Slit-lamp examination for Lisch nodules
Visual field testing
Hearing Tests:
Hearing tests and brainstem auditory evoked responses (especially in NF2)
Cognitive Assessment:
Neuropsychology review for learning or attention disorders
4. Management
Multidisciplinary Approach:
Neurology, Dermatology, Genetics, Ophthalmology, ENT, Orthopaedics, Psychology
Symptomatic & Surveillance Management:
Cutaneous neurofibromas: surgical excision if disfiguring or painful
Plexiform neurofibromas: monitor for malignancy (pain, rapid growth, neurological deficit → MRI + biopsy)
Optic glioma: observation vs. chemotherapy if progressive
Hearing loss (NF2): hearing aids, cochlear or auditory brainstem implants
Orthopaedic: correction of scoliosis or bone deformities
Psychological support for appearance and learning issues
Surveillance:
Annual skin, neurological and ophthalmic review
MRI brain/spine every 1–2 years (esp. in NF2)
Blood pressure monitoring (pheochromocytoma risk)
Family screening and genetic counselling
Novel Therapies:
MEK inhibitors (Selumetinib) for symptomatic, inoperable plexiform neurofibromas (NF1)
Neurofibroma Cheat Sheet
| Domain | NF1 | NF2 |
|---|---|---|
| Genetics / Aetiology | AD, mutation on chromosome 17 (NF1 gene) encoding neurofibromin | AD, mutation on chromosome 22 (NF2 gene) encoding merlin/schwannomin |
| Epidemiology | 1 in 3,000; 50% sporadic | 1 in 25,000; 50% sporadic |
| Key Features | ≥6 café-au-lait spots, axillary/inguinal freckling, ≥2 neurofibromas (or 1 plexiform), optic glioma, Lisch nodules, osseous lesion, or 1st-degree relative | Bilateral vestibular schwannomas ± meningiomas, ependymomas, cataracts |
| History | Skin lesions, learning difficulties, visual symptoms | Hearing loss, tinnitus, balance disturbance, seizures |
| Examination | Café-au-lait macules, cutaneous neurofibromas, Lisch nodules, scoliosis | Cranial nerve deficits, decreased hearing, schwannomas, meningiomas |
| Differentials | McCune-Albright, Tuberous sclerosis, Legius syndrome | Sporadic vestibular schwannoma, meningiomatosis |
| Investigations | Clinical criteria + MRI + genetics | MRI brain/spine + hearing tests + genetics |
| Management | Symptomatic, excision, MEK inhibitor, annual surveillance | Surgical removal of tumours, auditory implants, MRI surveillance |
| Complications | Malignant peripheral nerve sheath tumour, learning difficulty, scoliosis, hypertension | Deafness, brainstem compression, cranial neuropathies |